Shingles, medically known as herpes zoster, is a condition that can emerge unexpectedly, bringing with it significant discomfort and a distinctive rash. This often-intense experience typically manifests as a cluster of small, fluid-filled blisters on a red, inflamed area of skin, frequently accompanied by a sharp, burning pain. The discomfort can be so severe that it disrupts sleep, daily activities, and overall well-being, especially when the rash encircles one side of the body like an unwelcome band. It’s common for individuals to feel frustrated as this pain persists, often years after a childhood bout of chickenpox. However, gaining a clear understanding of shingles, its origins, and practical management strategies can empower you to navigate its challenges more effectively.
What Exactly Is Shingles?
Shingles develops when the varicella-zoster virus (VZV), the very same virus responsible for chickenpox, reactivates after lying dormant within your nerve tissues for many years. Reputable health organizations, including the CDC and Mayo Clinic, confirm that following a chickenpox infection (even a mild one you might not recall), the virus remains inactive until triggered. This trigger is often linked to the natural decline in immune function that occurs with age. The reactivation process leads to inflammation along a specific nerve pathway, which then results in the characteristic painful rash and associated nerve sensations. Studies indicate that while anyone who has had chickenpox can develop shingles, it is significantly more prevalent in adults over the age of 50.
Recognizing the Early Warning Signs
Before the visible rash of shingles makes its appearance, many individuals experience subtle yet crucial warning signals. These prodromal symptoms can last for several days and may sometimes be mistaken for other ailments like muscle strain or general nerve irritation. Key indicators to watch for include:
- A deep, burning, aching, or shooting pain in a localized area
- Tingling, itching, or an increased sensitivity to touch on the skin
- General malaise, such as fatigue, headache, or a mild fever
A critical distinguishing factor during this stage is the one-sided pattern of these sensations; shingles rarely extends across the body’s midline. Paying close attention to these early signs can be vital for timely intervention.
How the Shingles Rash Develops
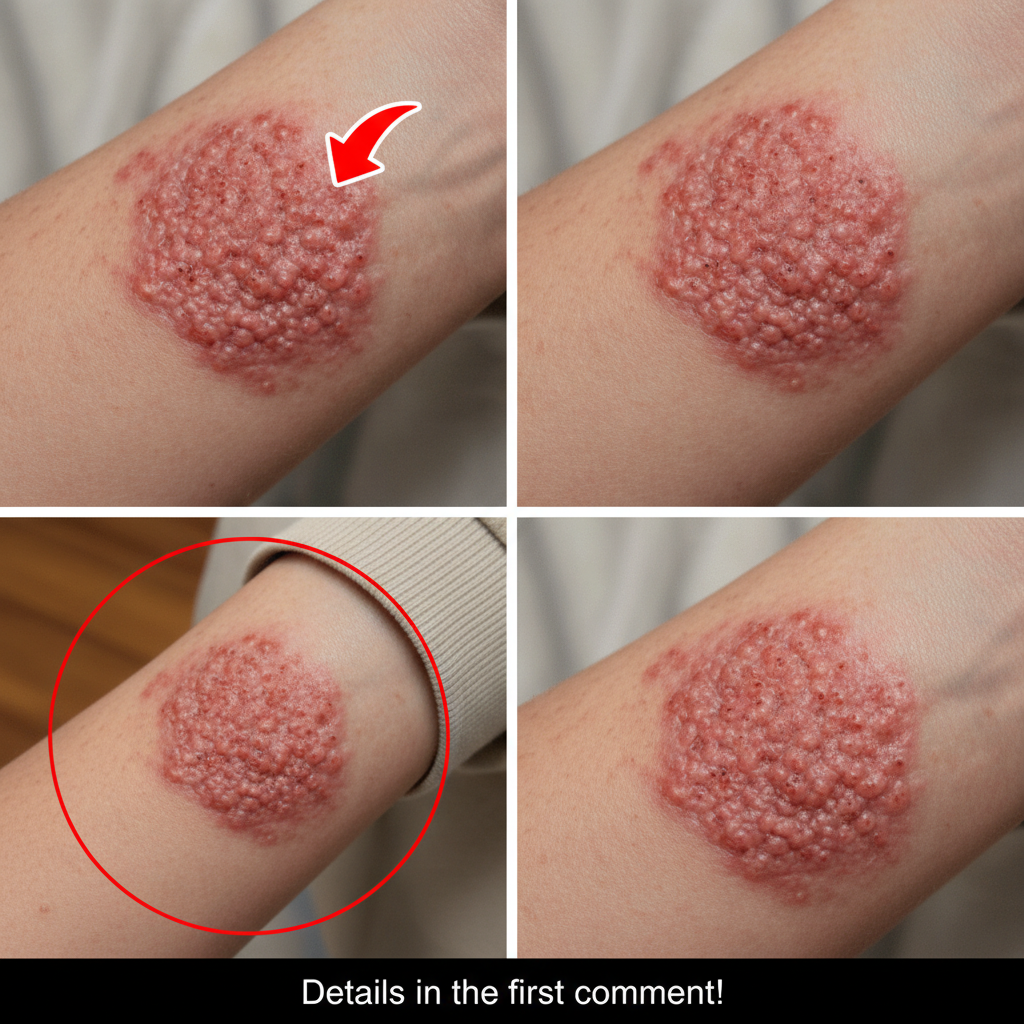
Following the initial prodromal phase, the most recognizable aspect of shingles emerges: the rash itself. It typically begins as red patches on the skin, soon followed by the formation of clusters of small, fluid-filled blisters. These blisters often resemble tiny bubbles on an inflamed base. Over the course of several days, these vesicles may rupture, ooze fluid, and eventually crust over. The entire rash frequently follows a distinct band-like or belt-shaped pattern, usually confined to one side of the torso, face, neck, or limbs. Common areas where the shingles rash can appear include:
- Around the waist or chest (often referred to as the classic “shingles belt”)
- On one side of the face or near the eyes
- The back, arms, or legs
The healing process for the rash generally takes between two to four weeks, although the affected skin area can remain sensitive or painful for an extended period. Research underscores that prompt recognition of these symptoms and early medical consultation can significantly improve management outcomes.
Why Does Shingles Reactivate? Common Risk Factors
Several factors can increase the likelihood of the dormant varicella-zoster virus becoming active again. According to leading health authorities, the primary risk factors for shingles reactivation include:
- Age: The risk of developing shingles increases dramatically after the age of 50, as the immune system naturally weakens with advancing years.
- Weakened Immunity: Any condition or treatment that compromises the immune system can trigger reactivation. This includes chronic stress, significant fatigue, certain illnesses (like HIV/AIDS or cancer), and medications that suppress the immune response (e.g., steroids, chemotherapy).
- Previous Chickenpox Infection: Nearly everyone born before the widespread availability of the chickenpox vaccine was exposed to the virus, making them susceptible to shingles later in life.
Understanding these triggers empowers individuals to focus on maintaining a healthy lifestyle and taking proactive steps to support their immune health.
Everyday Ways to Support Your Comfort During Shingles
While professional medical guidance is indispensable for managing shingles, several practical steps can help alleviate daily discomfort and promote healing at home:
- Keep the Affected Area Clean and Protected: Gently wash the rash with mild soap and water, then pat it dry. Avoid rubbing to minimize irritation. Loose-fitting clothing can also prevent friction.
- Apply Cool Compresses: A soft, damp cloth applied to the rash can provide soothing relief from burning sensations for short periods.
- Use Over-the-Counter Options Thoughtfully: Calamine lotion or colloidal oatmeal baths can help reduce itching and irritation for some individuals. Always follow product instructions.
- Prioritize Rest: Allow your body ample time to recover by reducing stress and maintaining a consistent, restorative sleep schedule.
- Stay Hydrated and Eat Nutrient-Rich Foods: Supporting your overall well-being with a balanced diet and sufficient fluid intake can aid the healing process.
These simple actions can contribute to a more comfortable environment while your body fights off the virus.
Prevention Insights: The Role of Vaccination
One of the most effective strategies for preventing shingles and its potential complications is vaccination. Health organizations, including the CDC, strongly recommend the recombinant zoster vaccine for all healthy adults aged 50 and older. It is also advised for younger adults facing certain immune challenges. Clinical studies have consistently shown that this vaccine can significantly lower the chances of developing shingles and reduce the severity and duration of symptoms if an outbreak does occur, as well as significantly decreasing the risk of post-herpetic neuralgia (persistent nerve pain). Discussing vaccination options with a healthcare provider is a proactive and highly recommended step.
When Should You Reach Out for Help?
Prompt medical attention is crucial for effective shingles management and to prevent potential complications. Contact a doctor without delay if you notice any of the following:
- A rash that appears near the eye or on the face, which could affect vision.
- Widespread or unusually severe symptoms.
- Persistent, worsening pain or signs of a secondary bacterial infection (e.g., increased redness, swelling, pus, fever).
Early consultation with a healthcare professional often leads to more effective management strategies and better long-term outcomes for individuals experiencing shingles.