Shingles, medically known as herpes zoster, often emerges unexpectedly, bringing with it significant discomfort and a distinctive visual presentation. This viral infection typically manifests as a cluster of small, fluid-filled blisters on a red, inflamed skin patch, frequently accompanied by a sharp, burning pain. This intense nerve pain can severely disrupt sleep, daily routines, and overall well-being, particularly when the rash encircles one side of the body. Many find themselves puzzled by its appearance, years after a childhood bout of chickenpox. The good news is that grasping the fundamentals of shingles, coupled with practical self-care measures, can profoundly improve how you cope with this challenging condition.
What Exactly Is Shingles?
At its core, shingles is caused by the reactivation of the varicella-zoster virus (VZV) – the very same virus responsible for chickenpox. After an initial chickenpox infection, even one so mild you might not recall it, VZV doesn’t leave your body. Instead, it retreats and lies dormant within your nerve tissues, sometimes for decades. Trusted health organizations like the CDC and Mayo Clinic confirm that this slumbering virus can reawaken due to various triggers, most commonly a natural decline in immune system effectiveness as we age. When reactivated, the virus travels along a nerve pathway, causing inflammation and leading to the hallmark painful rash and associated nerve sensations. While it can affect anyone who has had chickenpox, research consistently shows a higher incidence in adults over 50.
Recognizing the Early Warning Signs
Even before the distinctive shingles rash becomes visible, many individuals experience a set of subtle yet crucial early warning signs, often referred to as prodromal symptoms. These can manifest as:
- An intense, often deep-seated, burning, throbbing, or shooting nerve pain in a localized region.
- Unusual tingling, itching, or an extreme sensitivity to touch on a specific patch of skin.
- Systemic symptoms like general fatigue, a mild headache, or a slight fever.
These preliminary signs can persist for several days and are frequently misidentified as other conditions, such as a strained muscle or general nerve irritation. A critical indicator to watch for is the one-sided nature of these sensations – shingles almost invariably affects only one side of the body, rarely extending across the midline. But the journey of the rash doesn’t end there…
How the Shingles Rash Develops
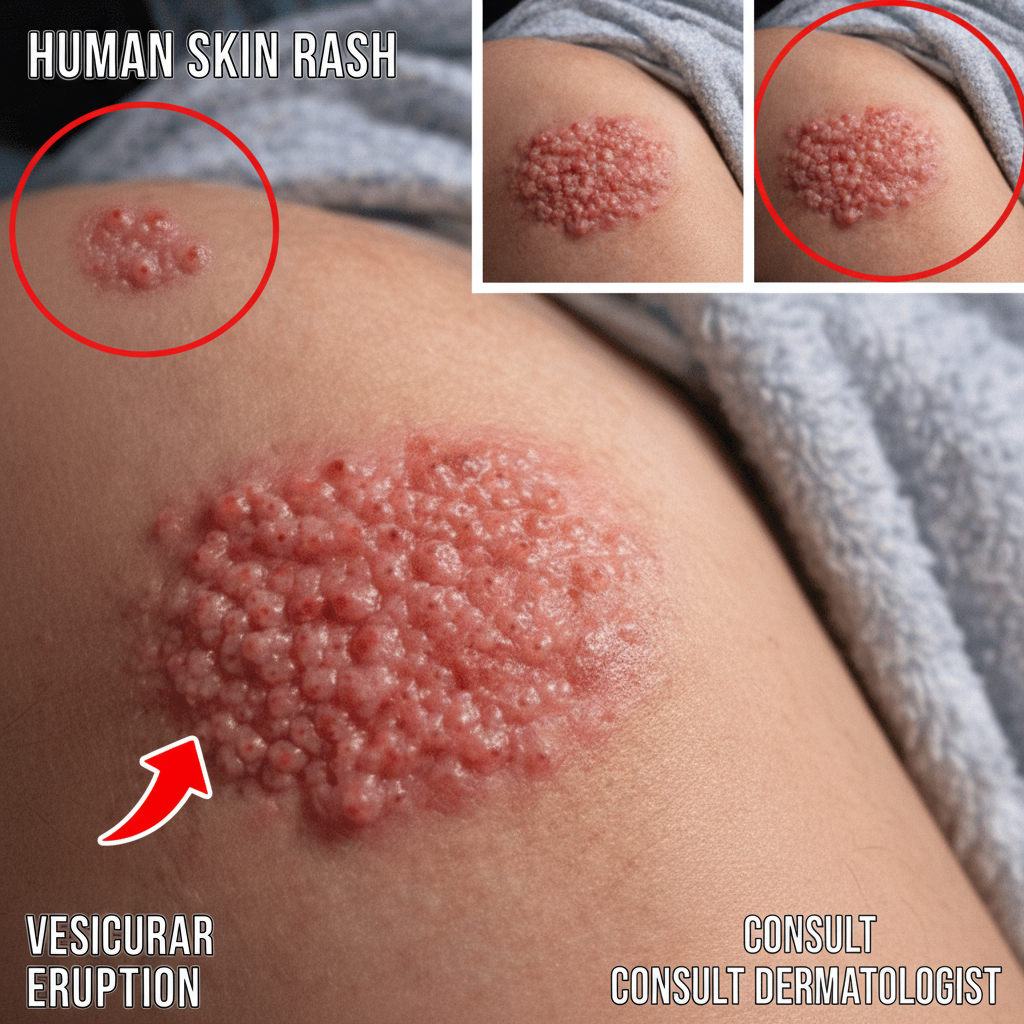
Following the initial discomfort, the characteristic shingles rash emerges. It typically begins as red, irritated patches of skin, quickly evolving into clusters of small, fluid-filled blisters. These blisters resemble tiny, clear bubbles set upon an inflamed, reddened base. Over the course of several days, these vesicles may rupture, weep fluid, and ultimately form scabs or crusts. The entire eruption commonly follows a distinct band-like or belt-shaped pattern, confined to one side of the body along a specific nerve pathway. Areas frequently affected include:
- The torso or chest, often forming the classic ‘shingles belt’ around the waistline.
- One side of the face, potentially extending to areas near the eyes.
- The back, arms, or legs.
While the rash generally takes 2 to 4 weeks to heal, the affected skin can remain tender and sensitive for some time afterward. Studies underscore the significant benefit of early recognition, as it facilitates prompt medical consultation and potentially more effective management.
Why Does Shingles Reactivate? Common Risk Factors
The dormant varicella-zoster virus can be stirred into activity by several contributing factors. Health authorities point to these common risk factors for shingles reactivation:
- Age: The most prominent risk factor, with the likelihood of developing shingles increasing substantially after the age of 50, primarily due to the natural age-related decline in immune system efficiency.
- Weakened Immune System: Any condition or circumstance that compromises the immune system can trigger reactivation. This includes chronic stress, periods of intense fatigue, certain medical illnesses (like cancer or HIV), or medications (such as corticosteroids or immunosuppressants) that suppress immune responses.
- Prior Chickenpox Infection: Crucially, shingles can only develop in individuals who have previously had chickenpox. Virtually everyone born before the era of widespread chickenpox vaccination was exposed to the virus, making them susceptible to reactivation.
Recognizing these potential triggers can help individuals focus on maintaining supportive habits and discussing preventive measures.
Everyday Ways to Support Your Comfort During Shingles
While seeking professional medical advice for shingles management is paramount, several practical everyday strategies can significantly alleviate discomfort and support your recovery:
- Maintain Cleanliness and Protection: Gently cleanse the affected skin area with mild soap and lukewarm water, then pat it dry thoroughly. Keeping the rash clean helps prevent secondary infections and minimizes irritation.
- Soothe with Cool Compresses: Applying a soft, damp, cool cloth to the affected area for short intervals can provide temporary relief from the burning and itching sensations associated with the shingles rash.
- Thoughtful Use of Over-the-Counter Aids: Certain over-the-counter products, such as calamine lotion or colloidal oatmeal baths, may offer some relief from itching and skin irritation. Always follow product instructions and consult your doctor if unsure.
- Prioritize Rest and Stress Reduction: Adequate rest is crucial for your body to combat the virus and heal. Minimize stress, and aim for a consistent sleep schedule to support your immune system.
- Nourish Your Body: Staying well-hydrated and consuming a balanced diet rich in essential nutrients can bolster your overall well-being and aid in the healing process.
Incorporating these supportive actions can foster a more comfortable environment as your body works to overcome the varicella-zoster virus.
Prevention Insights: The Role of Vaccination
A cornerstone of shingles prevention is vaccination. This topic is widely discussed and emphasized by global health organizations. The CDC, for instance, strongly recommends the recombinant zoster vaccine for all healthy adults aged 50 and older. It is also advised for younger adults facing specific immune system challenges. Extensive studies have consistently demonstrated that this vaccine can dramatically reduce both the risk of developing shingles itself and the severity of its complications, such as debilitating postherpetic neuralgia (prolonged nerve pain after the rash clears). Engaging in a conversation with your healthcare provider about appropriate vaccination options is a highly proactive and beneficial step for prevention.
When Should You Reach Out for Help?
While many cases of shingles can be managed with general medical care, certain situations warrant immediate attention from a healthcare professional. You should contact a doctor promptly if you observe any of the following:
- The rash appears near an eye or on the face, as this could lead to vision loss or other severe complications.
- The rash is widespread or particularly severe, indicating a potentially more serious infection.
- You have a weakened immune system due to illness or medication, as your body may struggle to fight the virus effectively.
- The pain is excruciating and unmanageable with typical pain relievers.
- You experience any signs of infection, such as increasing redness, warmth, swelling, or pus from the blisters.
Early intervention, especially in these circumstances, can prevent serious health issues and improve outcomes for shingles sufferers.