You’ve noticed a change—your mom seems a little more hunched, perhaps wincing with a persistent backache she dismisses as ‘just getting older.’ It’s tough to witness a loved one struggle, especially when it impacts cherished moments like embracing grandchildren or enjoying a leisurely stroll. But what if there’s a deeper reason behind her discomfort than simply the passage of time? This article will delve into the critical link between menopause and significant shifts in bone health, which could very well explain these symptoms. We’ll also cover practical, actionable habits to consider. Stay with us—by the end, you’ll discover not only key insights but also an unexpected daily routine that could profoundly support her well-being.
Understanding Osteoporosis: What It Is and Why Women Are More Vulnerable
Osteoporosis is a medical condition characterized by bones becoming progressively weaker and more brittle over time. This increased fragility makes them susceptible to fractures from even minor falls, bumps, or stresses that wouldn’t typically harm healthy bone. Our bodies constantly remodel bone tissue, replacing old cells with new ones. However, with osteoporosis, this delicate balance shifts, leading to a greater loss of bone mass than is regenerated.
Women, particularly after reaching menopause, face a significantly elevated risk of developing osteoporosis due to crucial hormonal changes. Statistics reveal that approximately half of all women over the age of 50 will experience a bone-related fracture during their lifetime. What makes this condition particularly insidious is its often ‘silent’ nature; it frequently progresses without noticeable symptoms until a fracture occurs, or until persistent issues like that nagging back pain become undeniable. Reputable studies consistently demonstrate a substantial decline in bone density during the perimenopausal and postmenopausal years. Think of your bones as a lifelong savings account: you diligently deposit density in your youth, but withdrawals accelerate significantly later in life. During menopause, this process speeds up dramatically, often contributing to changes in posture and chronic discomfort. The truth is, many people unfortunately attribute these signs to normal aging, but understanding the fundamental mechanisms can empower proactive steps.
The Pivotal Connection Between Menopause and Bone Health
Menopause marks a natural biological transition, typically occurring around age 51, signifying the end of menstrual cycles and a dramatic reduction in ovarian estrogen production. Estrogen is a vital hormone that plays a protective role in maintaining bone health by helping to preserve bone density. When estrogen levels plummet, the rate of bone breakdown begins to outpace bone rebuilding, resulting in bones that are thinner, less dense, and inherently more fragile.
This decline in estrogen commences during perimenopause and intensifies significantly post-menopause. Some women can experience a rapid loss of up to 20% of their bone mass within the first 5-7 years following menopause. Beyond hormonal shifts, several other factors can compound this risk, including a family history of osteoporosis, naturally low body weight, or the use of certain medications. For instance, if your mom experienced early menopause or underwent surgical removal of her ovaries, her risk profile would be elevated. It’s worth noting that while men also experience age-related bone loss, women’s typically smaller bone structures and longer lifespans make them more profoundly affected. Consider the spine, a complex stack of vertebrae supporting daily weight; weakened bones in this area can lead to painful compression fractures, resulting in the characteristic stooped posture known as kyphosis. Research consistently highlights that low estrogen is a primary driver of bone loss, but lifestyle choices undeniably play a crucial supporting role.
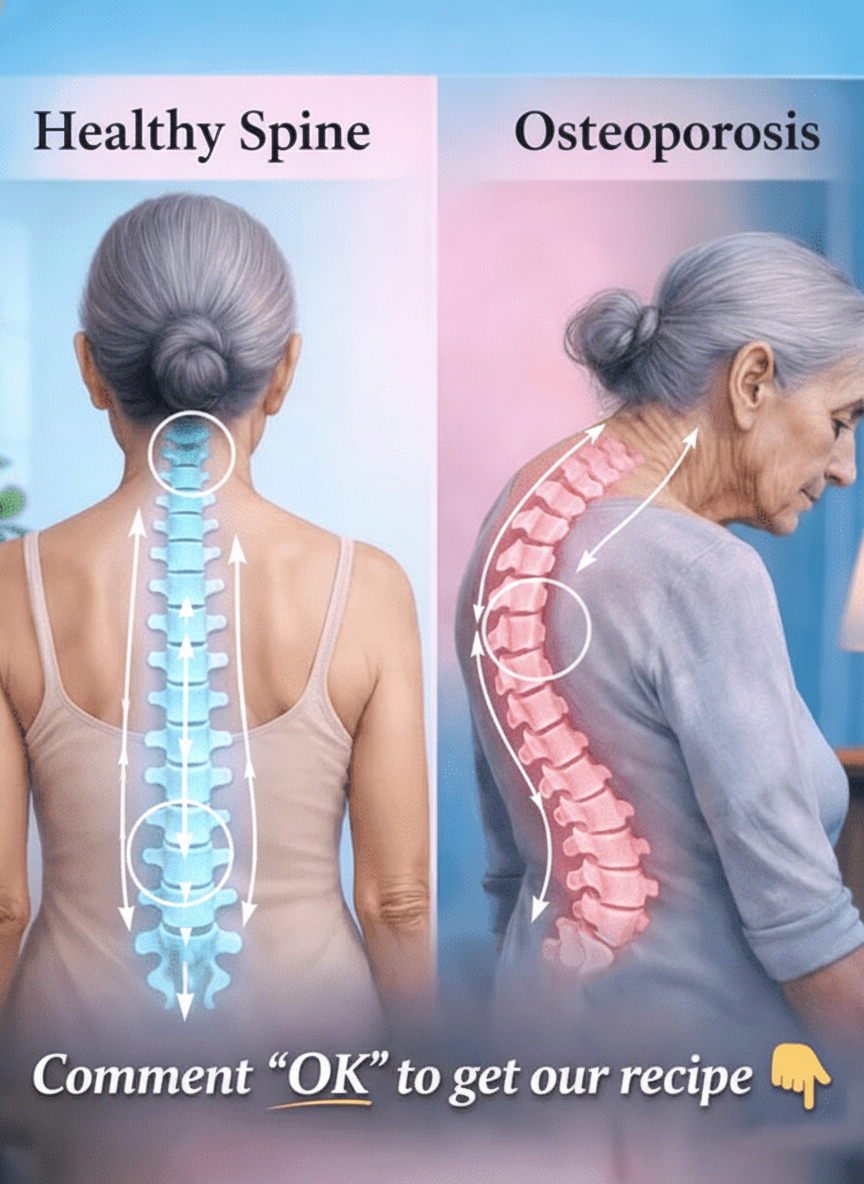
Recognizing the Common Signs of Potential Bone Issues
Chronic back pain is a very frequent complaint among individuals with osteoporosis, often stemming from tiny, unnoticed fractures within the spinal vertebrae that occur without a significant injury. Your mom might also observe a noticeable decrease in her height over time as these vertebrae gradually compress. Other telltale indicators include a progressively curved upper back, medically termed kyphosis or a “dowager’s hump,” or an increased susceptibility to bruising or fracturing bones from seemingly minor falls. However, it’s crucial to understand that these signs aren’t always immediately apparent; many individuals only receive an osteoporosis diagnosis after experiencing a more serious event, such as a hip or wrist fracture. Studies suggest that postmenopausal women are four times more likely than men to develop this condition. The consequences can extend to increased fatigue, limited mobility, and a significant impact on daily life and independence. Ignoring these subtle warnings could unfortunately lead to more severe complications, but recognizing them empowers you to take proactive and supportive steps.
Key Risk Factors for Osteoporosis During Menopause
Several elements can significantly heighten the risk of osteoporosis as women navigate menopause. Being aware of these factors can facilitate more informed discussions about your mom’s health:
- Age: As we grow older, the natural process of bone renewal slows down considerably.
- Ethnicity: Women of White or Asian descent generally have a higher predisposition to osteoporosis.
- Inadequate Calcium Intake: A lifelong deficiency in dietary calcium significantly compromises bone mineral density.
- Sedentary Lifestyle: A lack of regular weight-bearing exercise weakens bones over time.
- Smoking and Excessive Alcohol Consumption: Both habits can interfere with the body’s ability to form new bone tissue and absorb vital nutrients.
- Family History: Having a parent or close relative who suffered from osteoporosis or hip fractures increases personal risk.
- Certain Medications or Medical Conditions: Some hormone treatments for other conditions, as well as specific medical issues (e.g., thyroid disorders, certain gastrointestinal diseases), can also influence bone health.
Empowering Bone Health Through Lifestyle Habits
Implementing strategic lifestyle adjustments can make a profound and positive difference in maintaining and even improving bone strength, particularly for women during and after menopause. Here’s how to support robust bone health:
- Optimize Nutrition: Prioritize foods rich in calcium, such as dairy products (milk, yogurt, cheese), leafy green vegetables (kale, spinach, broccoli), and fortified items (cereals, orange juice).
- Ensure Adequate Vitamin D: Vitamin D is absolutely essential for the body to effectively absorb calcium. Obtain it through safe sun exposure, dietary sources like fatty fish (salmon, mackerel, tuna), or through supplements if dietary intake is insufficient. Research consistently shows that sufficient intake of both calcium and Vitamin D is crucial for bone mineral density.
- Engage in Regular Weight-Bearing Exercise: Activities like walking, jogging, dancing, and climbing stairs help stimulate bone formation and improve bone density.
- Incorporate Strength Training: Lifting weights or using resistance bands can build muscle mass and put beneficial stress on bones, further strengthening them.
- Limit Harmful Habits: Reduce or eliminate smoking and excessive alcohol consumption, as both negatively impact bone metabolism.
- Consider an Unexpected Daily Routine: While often overlooked, practicing mindful movement or gentle yoga daily can improve balance and flexibility, significantly reducing the risk of falls—a major cause of fractures in individuals with osteoporosis. Furthermore, consistent hydration and adequate sleep contribute to overall cellular health, indirectly supporting bone strength.