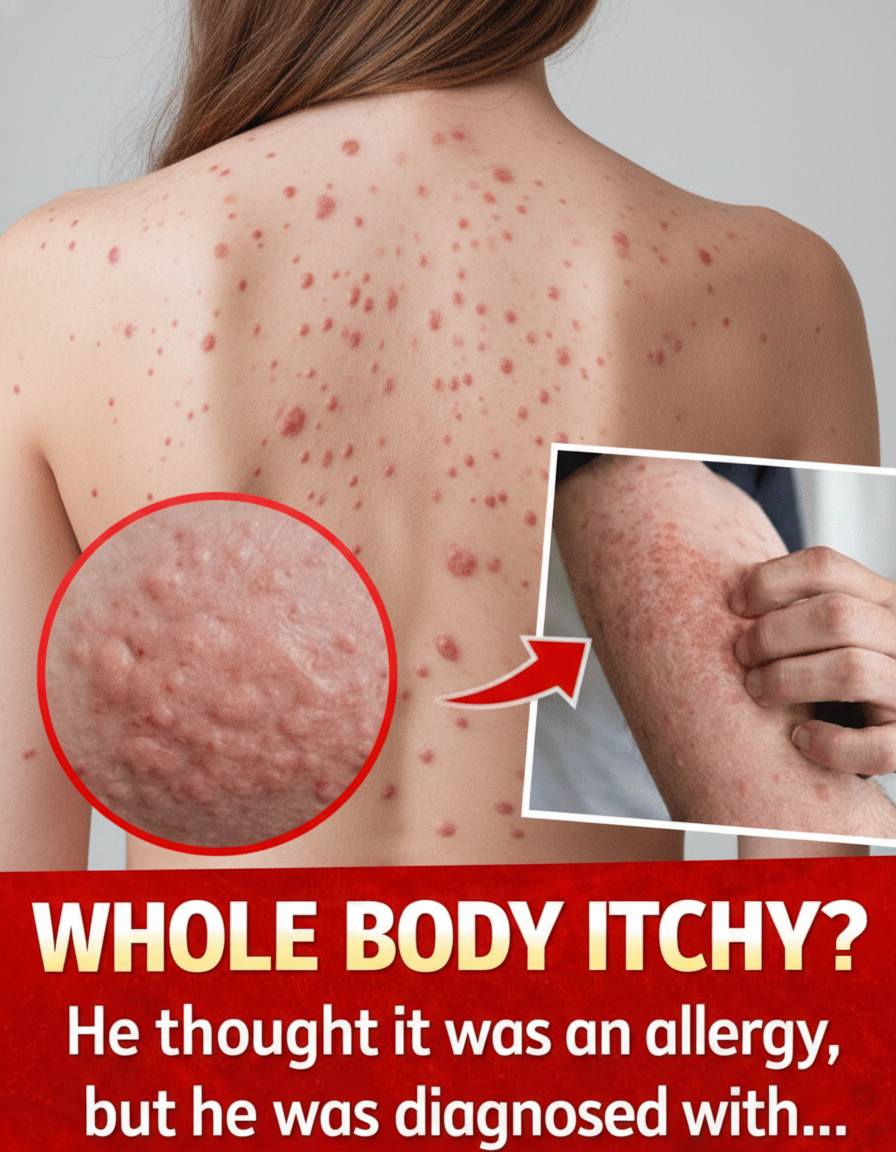
Picture experiencing an unyielding, full-body itch. Everywhere you look, angry red bumps emerge, transforming simple daily tasks into agonizing struggles. Naturally, you might presume it’s nothing more than a common allergy – perhaps triggered by certain foods, a new laundry detergent, or environmental factors. You might reach for readily available over-the-counter solutions, desperately seeking immediate relief. Yet, the irritation only intensifies, interfering with your sleep and overall quality of life. But what if this relentless itching is a symptom of something far more complex than a mere allergic response?
This exact predicament is encountered by countless individuals who dismiss extensive skin irritation as “just allergies.” However, experiences like the one highlighted in our story – where a visit to a medical professional unearths an unforeseen diagnosis – underscore the critical importance of heeding persistent bodily signals. Within this article, we will delve into the reasons why widespread itching and skin eruptions are frequently confused with allergic reactions, examine prevalent underlying causes, and offer actionable strategies to alleviate discomfort, all while emphasizing when expert medical consultation becomes indispensable. Stay tuned, as the most compelling revelations await towards the conclusion.
Why Persistent Itching and Red Bumps Are Frequently Mistaken for Allergies
The presence of widespread, intensely itchy, and inflamed red bumps across the skin can be profoundly distressing. The body’s immediate inflammatory response often results in elevated lesions that provoke an irresistible urge to scratch. Dermatological studies consistently reveal that numerous skin conditions initially manifest with strikingly similar symptoms, making an allergic reaction the default explanation for many. Allergic responses typically involve the release of histamine, leading to the formation of urticaria – those characteristic red, swollen, and transient welts. However, a range of other health issues can closely imitate this pattern.
Evidence suggests that incorrectly attributing these symptoms can significantly postpone an accurate diagnosis and appropriate treatment, thereby extending periods of discomfort. The reality is that not every itchy eruption originates from an allergen. Various factors, including bacterial or viral infections, exposure to environmental irritants, or even microscopic parasitic infestations, are capable of producing almost identical visible signs. This significant overlap clarifies why a great many individuals – much like the central figure in our narrative – initially conclude they are suffering from an allergy, only to discover a different underlying cause later on.
Common Conditions That Mimic Allergic Reactions
A number of distinct skin conditions can manifest as red, elevated, and intensely itchy eruptions across the body. Below, we delve into some of the most prevalent ones frequently misidentified as straightforward allergies:
- Hives (Urticaria): These are distinct, raised red welts that emerge abruptly and can migrate across the skin. While often associated with specific triggers such as stress, temperature fluctuations, or certain foods, they can also become chronic without an identifiable cause.
- Eczema (Atopic Dermatitis): Characterized by dry, inflamed skin patches that provoke severe itching. During flare-ups, the skin becomes red and bumpy, commonly affecting skin creases or presenting in widespread areas.
- Contact Dermatitis: This condition results in itchy, red bumps developing after direct contact with irritants or allergens, including specific textiles, chemical cleansers, or plant substances.
- Viral Rashes: Various viral infections can induce widespread red spots or papules that cause itching. These can closely resemble allergic outbreaks but are intrinsically linked to the body’s immune response fighting off a virus.
- Scabies: A highly contagious infestation caused by microscopic mites burrowing into the skin. It leads to excruciating itching, which is often exacerbated at night, alongside small red bumps or tell-tale burrow tracks. Scabies is frequently misdiagnosed as eczema or an allergy due to the intense hypersensitivity reaction to the mites. Medical research underscores how scabies, in particular, is often overlooked because its severe pruritus can feel indistinguishable from an allergic reaction. One notable study documented instances where patients endured months of incorrect diagnoses before the true nature of their condition was accurately identified.
However, the narrative doesn’t end there. Crucial distinctions often emerge through careful observation of patterns, the timing of symptoms, and any additional accompanying signs.
Spotting the Differences: Allergic Reactions Versus Other Causes
To facilitate a clearer understanding, here’s a concise comparison of key indicators:
- Typical Allergic Reaction (Hives): Characterized by a rapid onset, with welts usually subsiding within a few hours to a couple of days. These often respond promptly to antihistamine medication.
- Eczema Flare-up: Involves chronic skin dryness, often leading to thickened skin over prolonged periods. There’s frequently a familial predisposition to allergies or asthma.
- Scabies Infestation: Marked by severe itching that typically intensifies during the night. Bumps commonly appear in skin folds (such as wrists, elbows, and groin), and faint, thread-like lines (burrows) might be visible. It spreads readily through close personal contact.
- Viral Exanthem (Rashes): May be accompanied by systemic symptoms like fever and fatigue. The spots could potentially evolve into blisters, and the rash generally resolves as the viral infection naturally runs its course.
If your itching endures despite diligently avoiding presumed triggers, or if it noticeably worsens during nighttime hours, these signs may strongly indicate an underlying condition beyond a simple allergic response.
Actionable Tips to Alleviate Discomfort While Awaiting Diagnosis
While awaiting a definitive diagnosis and guidance from a healthcare professional, implementing these evidence-based practices can significantly help manage symptoms and foster overall skin health:
- Maintain Skin Coolness and Hydration: Immediately after bathing, generously apply fragrance-free moisturizers to effectively seal in moisture. Utilizing cool compresses can also substantially reduce inflammation and provide soothing relief from persistent itching.
- Resist the Urge to Scratch: Although often easier said than done, preventing scratching is crucial. Keep nails meticulously trimmed, consider wearing soft cotton gloves during sleep to minimize inadvertent scratching, or indulge in cool oatmeal baths, which are known for their calming properties without compromising skin integrity. Breaking the skin through scratching can lead to secondary infections and further complications.
Ultimately, while these tips offer temporary respite, they are not a substitute for professional medical evaluation. If your persistent itching, redness, or bumps do not improve, or if they worsen, seeking advice from a dermatologist or general practitioner is paramount to uncover the true cause and embark on an effective treatment plan. Your skin health is a vital component of your overall well-being, and understanding its signals is the first step towards lasting relief.