Many women worldwide routinely experience monthly discomforts like menstrual cramps or general fatigue, often dismissing them as an inevitable part of life. However, when these symptoms persist, intensify, and significantly disrupt daily activities, they could indicate a more serious underlying condition: endometriosis. This prevalent issue affects millions globally, frequently leading to years of undiagnosed suffering because its symptoms often mimic those of common ailments, delaying crucial recognition. Imagine discovering subtle signals your body has been sending all along – stay with us, because at the end, we’ll share a simple tracking method that could profoundly change how you manage your health.
Why Endometriosis Symptoms Are Frequently Misunderstood and Overlooked
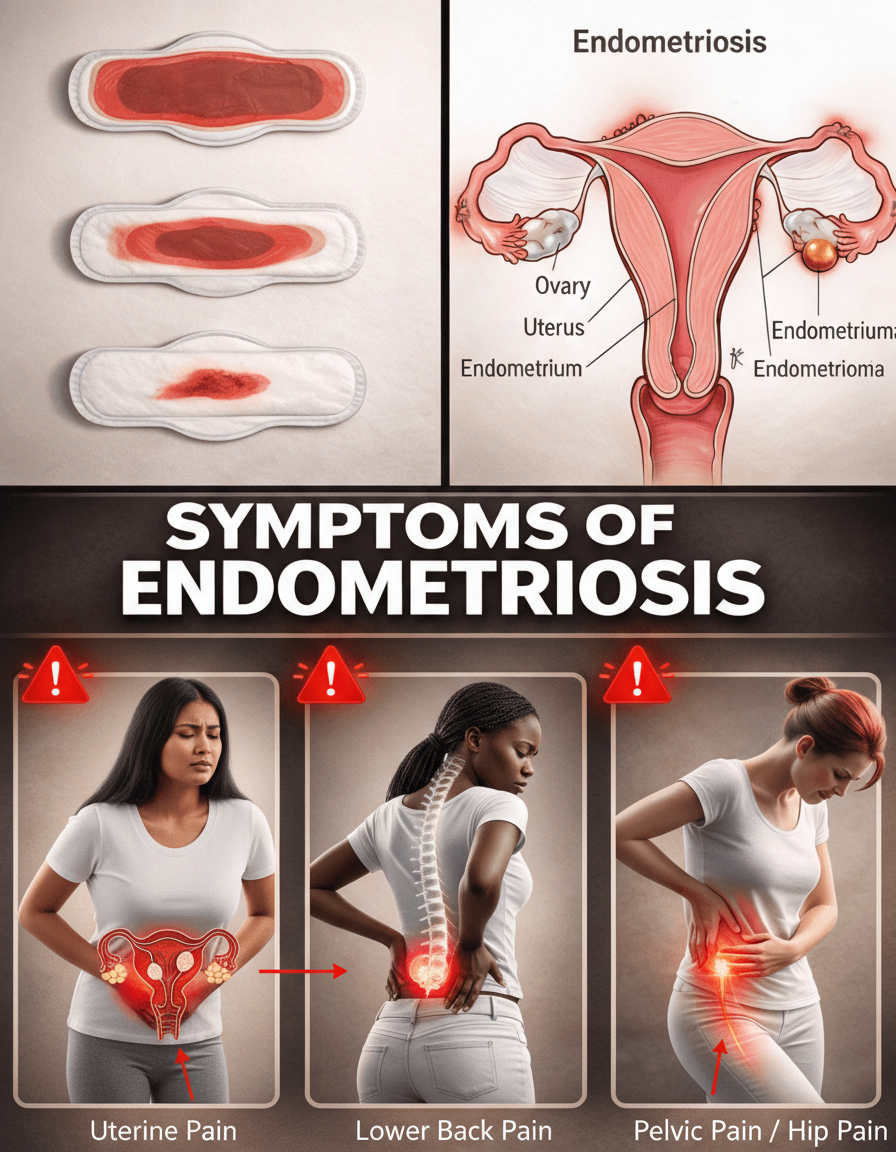
Endometriosis is characterized by the growth of tissue similar to the uterine lining outside the uterus itself, resulting in inflammation, pain, and sometimes scar tissue. According to reputable sources like the Mayo Clinic, this condition affects approximately 10% of women of reproductive age. Yet, obtaining an accurate diagnosis can unfortunately take an average of 7 to 10 years. A primary reason for this delay is that endometriosis symptoms often resemble everyday problems, such as premenstrual syndrome (PMS) or digestive upsets, making them easy to disregard. Furthermore, many women normalize these challenging experiences, believing them to be simply ‘part of being a woman.’ Research from the Cleveland Clinic highlights that while pain often begins cyclically, it can progressively become constant over time. The key takeaway here is that early awareness and recognition can profoundly impact daily life and long-term management. Let’s explore 13 crucial warning signs, starting with some of the most common indicators.
-
Excruciating Menstrual Cramps That Disrupt Your Life
Intense pelvic pain and cramping that begins before your period and persists for several days can be a critical indicator of endometriosis. This discomfort transcends typical period pain; it’s often described as debilitating, severe enough to cause missed work, school, or social activities. The Mayo Clinic identifies this agonizing pelvic pain, frequently accompanied by lower back or abdominal aches, as a hallmark symptom. If over-the-counter pain relievers offer little to no relief, it’s a significant sign to consider further investigation.
-
Persistent Pelvic Pain Unrelated to Your Menstrual Cycle
Beyond your monthly period, ongoing discomfort in the lower abdomen, pelvic region, or back that isn’t solely tied to menstruation can signal potential issues. This chronic pelvic pain often fluctuates and may even worsen with hormonal changes throughout the month. As noted by experts at the Cleveland Clinic, this persistent discomfort arises from continuous inflammation within the pelvic cavity. It might manifest as a constant, dull ache that significantly impacts your daily routine. While easily mistaken for stress or other common ailments, it’s crucial to consider other possibilities.
-
Discomfort During or After Intimacy
Experiencing deep-seated pain during or following sexual activity, often described as internal pressure, sharpness, or a burning sensation, is a common yet frequently overlooked symptom of endometriosis. This can profoundly affect personal relationships and often leads to avoidance of intimacy. Studies highlight how adhesions or scar tissue, which are common in endometriosis, can contribute significantly to this specific type of pain. If this discomfort leads to growing reluctance or apprehension, it’s a symptom that warrants immediate attention.
-
Unusually Heavy or Prolonged Menstrual Flow
Excessive menstrual bleeding that necessitates frequent changes of sanitary products (pads or tampons), along with the passage of large blood clots or periods that last significantly longer than seven days, can be a strong indicator of endometriosis. Additionally, intermenstrual spotting, or bleeding between cycles, may also occur. Health resources often link these abnormal bleeding patterns to potential hormonal imbalances or endometrial tissue within the uterine muscle itself (adenomyosis), which often coexists with endometriosis. It’s important to compare your experiences to what is considered typical for others.
-
Painful Bowel Movements or Urination During Periods
Experiencing discomfort, increased urgency, or outright pain during bowel movements or urination, particularly around your menstrual period, serves as another significant diagnostic clue. This can manifest as symptoms like cyclical diarrhea, constipation, painful straining, or even visible traces of blood in stool or urine. The presence of endometrial lesions on or near the bladder or intestines can be responsible for these cycle-dependent gastrointestinal and urinary issues. If your bathroom routines become noticeably challenging or painful during menstruation, it’s imperative to take notice.
-
Persistent, Debilitating Fatigue
A profound and pervasive sense of exhaustion or low energy, even following adequate rest, is a common symptom that often intensifies during menstruation. Many individuals with endometriosis report experiencing ‘brain fog,’ difficulty concentrating, and debilitating fatigue that interferes with their ability to function. Research consistently suggests that the chronic inflammation and systemic stress associated with endometriosis play a significant role in this pervasive tiredness. Imagine struggling through your days feeling utterly drained despite getting sufficient sleep.
-
Abdominal Bloating and Digestive Discomfort
Frequent abdominal swelling (often referred to as ‘endo belly’), nausea, or general digestive upset that cyclically worsens, particularly before or during your period, can mimic Irritable Bowel Syndrome (IBS) but is often connected to endometriosis. The severity of these gastrointestinal symptoms is typically attributed to the involvement of endometrial implants on or around the bowel. If you experience unusually uncomfortable, persistent, or cyclical bloating and digestive issues, it warrants thorough investigation.
-
Challenges with Conception and Infertility
Struggling to conceive after several months or more of trying is a significant concern for many, affecting up to 50% of women diagnosed with endometriosis-related infertility. The presence of inflammation, scar tissue, or adhesions caused by endometriosis can physically impede the reproductive process by distorting anatomy or affecting egg release and fertilization. The emotional toll of unexplained delays in getting pregnant is widely reported. If you find yourself in this situation, it’s a compelling reason to seek further evaluation for endometriosis.
-
Pain Radiating to the Lower Back, Hips, or Legs
Pain that radiates into the lower back, hips, or legs, sometimes mimicking sciatica, often originates from the chronic pelvic inflammation characteristic of endometriosis. This discomfort can be intermittent, occurring particularly during menstruation, or it can be a constant presence, significantly impacting mobility and comfort. Such symptoms suggest nerve involvement or the spread of endometrial lesions to areas outside the immediate pelvic cavity, potentially irritating nerves in the lumbar or sacral regions.
-
Nausea and Vomiting During Periods
Beyond general digestive upset, some women with endometriosis experience severe nausea, sometimes accompanied by vomiting, especially during their menstrual cycle. This can be linked to the release of prostaglandins (hormone-like substances that cause uterine contractions and inflammation) or the spread of endometrial lesions to parts of the gastrointestinal tract, intensifying systemic symptoms.
-
Painful Urination (Dysuria)
While often grouped with general urinary discomfort, painful urination (dysuria) that consistently flares during menstruation can be a specific sign. This occurs if endometrial implants are present on or near the bladder, causing inflammation and irritation when the bladder fills or empties. It’s crucial to distinguish this from a urinary tract infection (UTI), as it often presents without bacterial infection.
-
Allergies and Chemical Sensitivities
Though less commonly discussed, some individuals with endometriosis report an increased susceptibility to allergies, food sensitivities, and even chemical sensitivities. While the exact link is still being researched, it’s thought that the chronic inflammatory state and immune system dysregulation associated with endometriosis may contribute to these broader sensitivities, indicating a systemic impact beyond just pelvic pain.
-
Anxiety and Depression
Living with chronic, often debilitating pain and the frustration of delayed diagnosis can significantly impact mental health. Many women with endometriosis experience heightened levels of anxiety and depression, not just as a reaction to their condition, but potentially also due to the systemic inflammation and hormonal fluctuations that can influence mood-regulating neurotransmitters. Recognizing these mental health challenges as part of the overall picture is vital for comprehensive care.
Recognizing these 13 common warning signs is the first crucial step toward understanding your body and seeking appropriate care. If any of these symptoms resonate with your experiences, especially if they are severe, persistent, or significantly impact your quality of life, it is imperative to consult a healthcare professional. Don’t dismiss your symptoms as ‘normal.’ Early diagnosis and management can dramatically improve outcomes and quality of life for those living with endometriosis.
As promised, a simple tracking method can be incredibly helpful: start a symptom diary. Note down the dates, specific symptoms (pain levels, location, type of bleeding, digestive issues, fatigue, mood changes), their intensity, and how they relate to your menstrual cycle. This detailed record will provide invaluable information for your doctor, helping them connect the dots and accelerate your journey toward an accurate diagnosis and effective treatment plan. Your health journey begins with listening to your body.