Decoding Your Uterus: 12 Vital Signals You Should Never Ignore
Many women instinctively brush off subtle shifts in their bodies, attributing them to life’s stresses, aging, or just ‘being a woman.’ Yet, your uterus, a resilient and powerful organ, often sends quiet, crucial signals when something isn’t quite right. These aren’t just minor annoyances; they can be tied to common gynecological conditions like fibroids, endometriosis, or adenomyosis. Ignoring them can allow small, manageable issues to escalate into significant disruptions to your daily comfort, energy, and overall well-being.
The challenge? These warning signs often start subtly, feeling ‘normal’ until they intensify or combine, making everyday life difficult. The good news is that early awareness and a conversation with your healthcare provider can profoundly impact your reproductive health. Stay with me, as we’ll explore these signs and practical steps you can take to support your uterine health today.
What Your Uterus Might Be Trying to Tell You
Your uterus is a complex organ, and various conditions can affect its function, leading to noticeable changes. Research from reputable sources like the Mayo Clinic and Cleveland Clinic highlights that symptoms often overlap across different issues, including uterine fibroids (noncancerous growths), endometriosis (tissue similar to the uterine lining growing outside the uterus), and other pelvic concerns. Here are 12 common warning signs reported by women – pay close attention if they persist or worsen:
- Heavy or Prolonged Menstrual Bleeding: Periods that demand a pad or tampon change every hour, last longer than seven days, or involve large blood clots. This is a common indicator of conditions like fibroids or adenomyosis.
- Bleeding Between Periods or After Menopause: Any spotting or bleeding outside your regular cycle, especially post-menopause, is a significant red flag that warrants immediate medical attention.
- Severe Menstrual Cramps: Pain that is noticeably worse than usual, doesn’t respond well to over-the-counter pain relief, or begins days before your period and lingers afterwards.
- Pelvic Pressure or Fullness: A persistent sensation of heaviness or pressure in your lower abdomen, often described as bloating that just won’t go away.
- Pain During Intercourse: Discomfort or sharp pain experienced during or immediately after sexual activity, which can indicate issues like endometriosis or fibroids pressing on surrounding tissues.
- Frequent Urination or Difficulty Emptying the Bladder: An increased need to urinate, or feeling as though your bladder isn’t completely empty, often due to growths pressing on the bladder.
- Lower Back or Abdominal Pain: A chronic ache in the lower back, pelvis, or abdomen that isn’t solely tied to your menstrual cycle.
- Painful Bowel Movements or Constipation: Discomfort during bowel movements, or noticeable changes in bowel habits, particularly around your period.
- Unusual Vaginal Discharge: Any changes in the color, odor, consistency, or amount of discharge – watery, bloody, or foul-smelling discharge should be promptly investigated.
- Fatigue or Low Energy Tied to Cycles: Extreme tiredness, potentially stemming from heavy bleeding leading to anemia, which is a frequent companion to prolonged periods.
- Abdominal Bloating or Swelling: Your belly feeling larger or fuller, sometimes causing clothes to fit differently, even without any weight gain.
- Changes in Cycle Regularity: Periods becoming unpredictable, significantly shorter or longer, or skipping altogether – these can signal hormonal imbalances or structural changes within the uterus.
These signs rarely appear in isolation. When multiple symptoms overlap, it’s often your body’s clear message to seek professional guidance.
Understanding the ‘Why’: Common Uterine Conditions
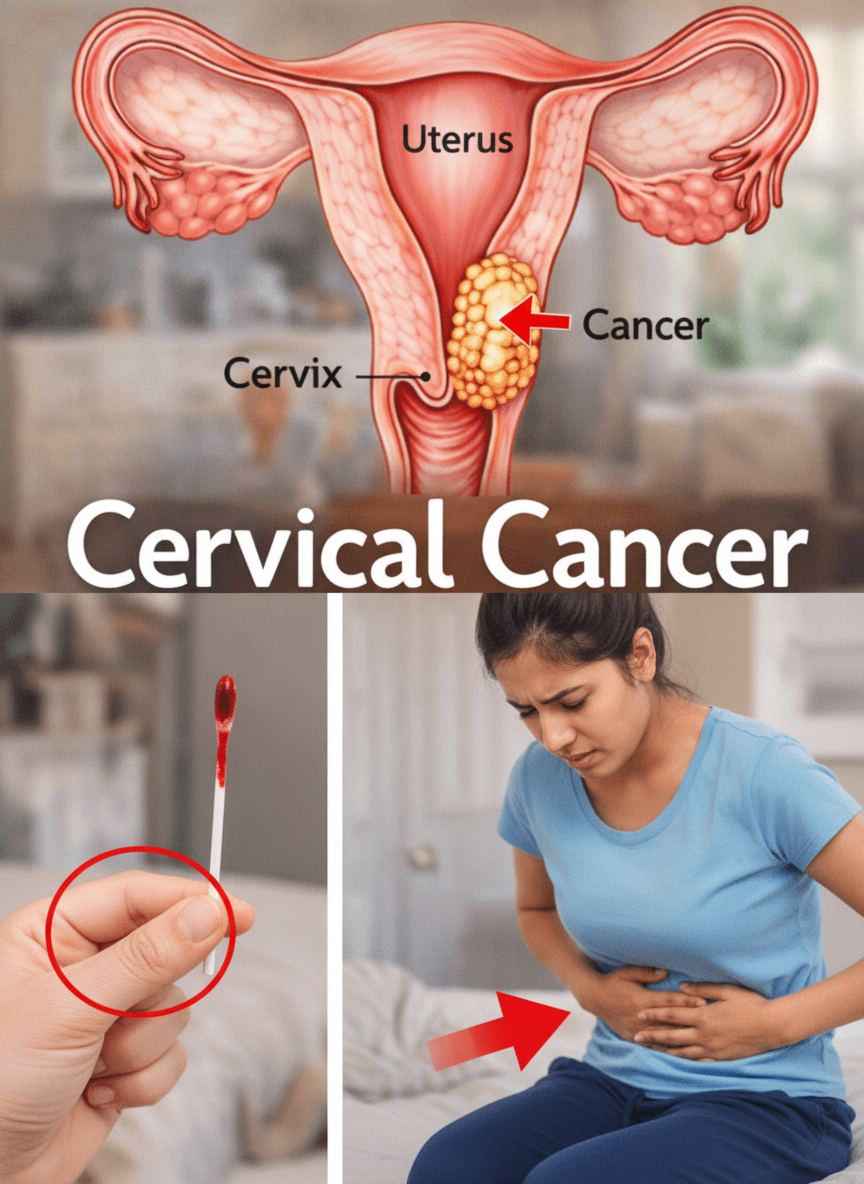
Many of these symptoms arise from benign (non-cancerous) conditions that affect millions of women globally. For instance:
- Uterine Fibroids: These non-cancerous growths can affect up to 80% of women by age 50 (per Cleveland Clinic data), often causing heavy bleeding, pain, and pressure.
- Endometriosis: Impacting approximately 10% of reproductive-age women (Mayo Clinic), this condition involves tissue similar to the uterine lining growing outside the uterus, leading to chronic pain and irregular cycles.
- Adenomyosis: Characterized by the uterine lining growing into the muscular wall of the uterus, this condition frequently results in heavy, painful periods.
The critical takeaway? Early awareness empowers you to have more informed conversations with your doctor. Regular check-ups, including pelvic exams and ultrasounds when necessary, are instrumental in identifying the root cause of your symptoms.
Proactive Steps for Uterine Wellness
You don’t have to wait for symptoms to worsen. Here are practical, everyday habits endorsed by health experts to support your uterine health:
- Track Your Cycle: Utilize an app or journal to meticulously log your periods, pain levels, flow, and any unusual symptoms. These detailed patterns provide invaluable data for your healthcare provider, helping them diagnose issues faster.
- Stay Hydrated and Eat Iron-Rich Foods: Especially if you experience heavy bleeding, maintaining good hydration and consuming iron-rich foods (like spinach, lentils, and lean meats) helps prevent anemia and supports overall energy levels.
Your body communicates with you constantly. By tuning into these vital signals from your uterus and acting proactively, you can maintain better reproductive health and enhance your overall quality of life. Don’t hesitate to reach out to a healthcare professional if you recognize any of these persistent warning signs.