Amlodipine Side Effects: What Seniors Need to Watch For
You’ve started your doctor-prescribed blood pressure medication, amlodipine, and after a few weeks, something feels… off. Your shoes are tighter, your head feels heavy, or a family member points out subtle facial swelling. Many older adults dismiss these changes as “just aging.” However, these uncomfortable symptoms might be linked to medications like amlodipine.
The good news? Most of these reactions are manageable once you know what to look for. And by the end of this article, you’ll discover a simple daily habit many doctors recommend for safely monitoring medication reactions.
Why Amlodipine is a Common Prescription
Amlodipine is a widely used medication that helps relax blood vessels, allowing blood to flow more easily throughout the body. This makes it a common choice for managing high blood pressure and improving circulation, often becoming a daily routine for adults over 50.
While calcium channel blockers like amlodipine have significantly helped millions maintain healthier blood pressure, it’s crucial to remember that every medication affecting the body can also have side effects. Most are mild and temporary, but understanding them empowers you to be a smarter observer of your own health. Let’s explore the most commonly reported changes.
Swelling in Feet and Ankles (Peripheral Edema)
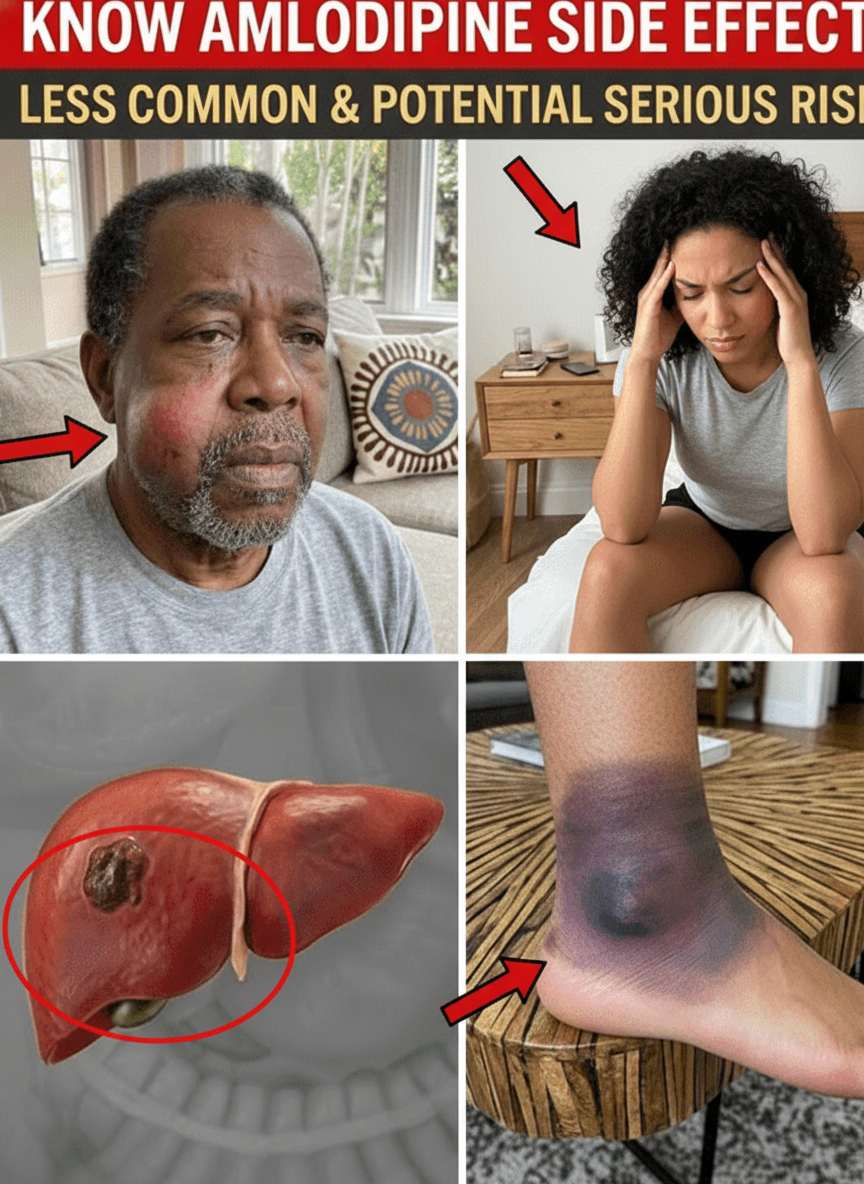
One of the most frequently reported side effects of amlodipine is swelling in the lower legs or ankles, often called peripheral edema. This occurs because amlodipine, while relaxing blood vessels to improve circulation, can also cause fluid to collect in the tissues around your feet and ankles.
You might notice this when:
- Your shoes feel suddenly tight in the evening.
- Socks leave deeper marks on your skin.
- Your ankles appear puffier after sitting for long periods.
Mild swelling is usually not dangerous, but sudden or severe swelling warrants immediate discussion with a healthcare professional. Simple daily habits can help reduce fluid buildup:
- Elevate your legs for 20 minutes in the evening.
- Stay gently active with short walks.
- Reduce excessive salty foods.
Headaches and Dizziness
If you’ve recently started amlodipine and experience occasional dizziness or mild headaches, you’re not alone. As blood vessels relax and blood pressure adjusts, your body needs time to adapt. During this adjustment phase, some individuals may experience:
- Lightheadedness when standing quickly.
- A dull pressure headache.
- Temporary fatigue during the afternoon.
These symptoms often improve as your body stabilizes. However, for older adults, dizziness increases the risk of falls. A simple, yet vital, precaution: Before standing up from a chair or bed, pause for a few seconds. Allow your body to adjust slowly. This small routine can prevent many accidents.
Facial Flushing and Warm Skin
Some individuals notice their face becomes warm or red shortly after taking amlodipine – a reaction known as flushing. This happens because blood vessels near the skin’s surface widen slightly, increasing blood flow to the face. You might experience:
- Warm cheeks.
- Mild redness across the face.
- A brief sensation of heat.
This feeling usually fades quickly. Interestingly, many people confuse flushing with embarrassment or stress, when it could simply be the medication working. If flushing becomes uncomfortable, drinking water and moving to a cooler environment often helps.
Digestive Changes Some People Notice
A smaller group of people taking amlodipine report digestive changes, including:
- Mild nausea.
- Stomach discomfort.
- Occasional constipation.
The digestive system can be sensitive to medications due to its interaction with circulation and fluid balance. A practical tip often recommended by clinicians: try taking your medication with food or at a consistent time each day to help minimize stomach upset.
Your Simple Daily Habit for Safer Medication Use
The most important step in managing any medication is proactive observation. Many doctors recommend a simple “body check-in” each day. Pay attention to how you feel, noting any new or unusual symptoms, no matter how minor. This could involve:
- Quickly scanning your body for swelling.
- Noticing any changes in energy or balance.
- Reflecting on your digestion.
If you observe any persistent or concerning changes, especially those mentioned above, communicate them clearly with your doctor or pharmacist. They can assess if the symptom is medication-related and adjust your treatment plan if necessary. Remember, understanding your body’s signals is key to a healthier life, especially when managing chronic conditions.