Endometriosis: Unmasking the Pain Many Women Overlook
You’re at the dinner table, a sudden wave of pelvic pain makes you shift, hoping no one notices. You might laugh it off, blaming it on “just another bad period.” But deep down, a nagging feeling tells you this pain is different – stronger, harder to ignore. Many women feel embarrassed discussing menstrual pain, yet this silence can allow a hidden condition like endometriosis to quietly disrupt daily life for years. The good news? Understanding early signals and adopting healthy habits can safeguard your long-term well-being and comfort.
What Is Endometriosis and Why Awareness Matters
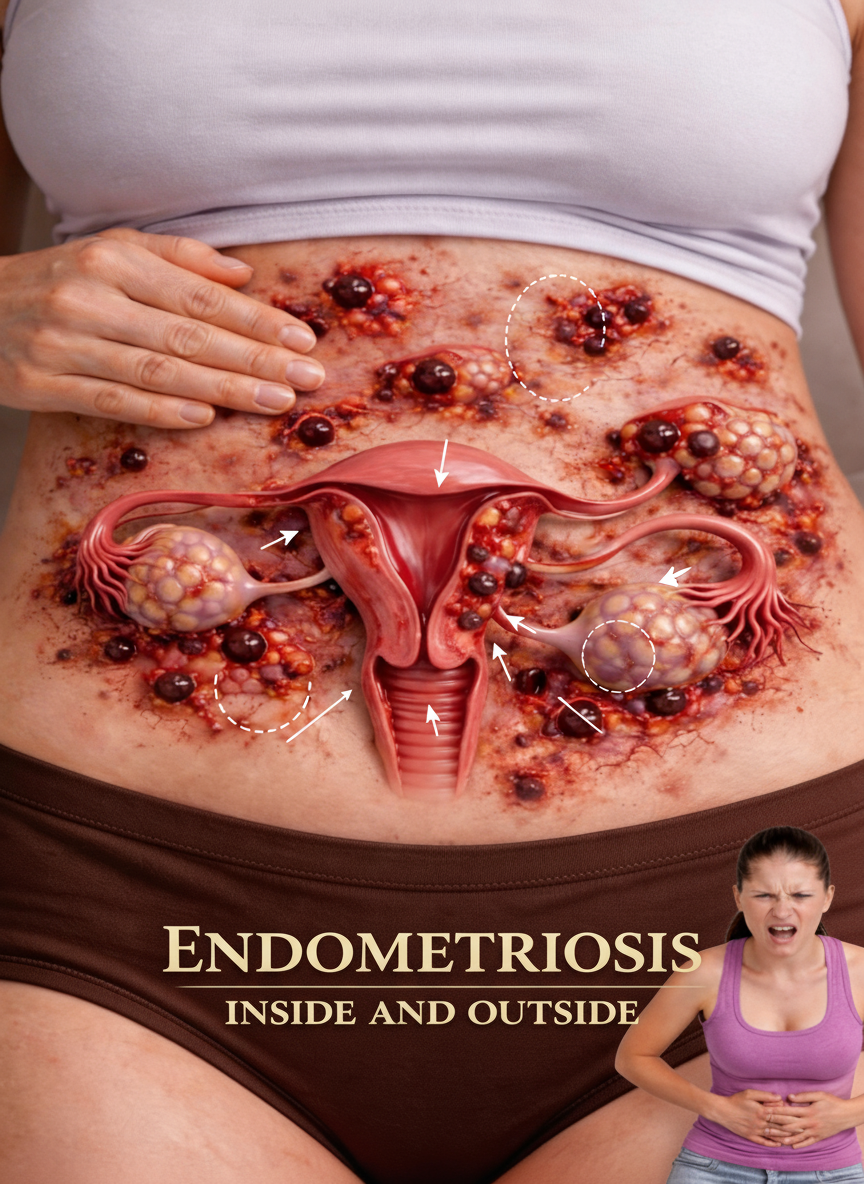
Endometriosis is a condition where tissue similar to the lining inside the uterus (endometrium) grows outside it. Common sites include the ovaries, fallopian tubes, and other pelvic areas. During your monthly hormonal cycle, this misplaced tissue behaves like uterine lining: it thickens and attempts to shed. However, unlike the uterine lining, it has no easy exit from the body. This leads to irritation, inflammation, and scar tissue in surrounding areas.
Alarmingly, reproductive health journals indicate millions worldwide live with endometriosis, often spending years dismissing their symptoms as “normal menstrual pain.” This delay significantly impacts daily comfort, mobility, and emotional well-being.
To better understand, consider this comparison:
- Normal Menstrual Cycle: Uterine lining builds and sheds monthly; menstrual blood exits through the cervix; mild to moderate cramping.
- Endometriosis-Related Changes: Tissue grows outside the uterus; tissue cannot exit normally; persistent pelvic discomfort or pressure.
Early recognition of these patterns and prompt consultation with healthcare professionals are crucial.
Common Symptoms Many Women Overlook
Symptoms vary widely, from intense discomfort to subtle changes, highlighting the importance of awareness. Keep an eye out for:
- Persistent pelvic discomfort
- Menstrual cramps that worsen over time or become debilitating
- Pain during or after sex, urination, or bowel movements
- Digestive issues (bloating, diarrhea, constipation) around menstrual cycles
- Unusual or chronic fatigue, especially during periods
- Lower back pain during menstruation
- Irregular menstrual patterns or heavy bleeding
- Pressure sensations in the pelvic area
Gynecological studies show that symptom intensity doesn’t always correlate with the amount of tissue growth; even small areas can cause significant discomfort. Listening closely to your body provides the earliest clues.
Possible Causes and Risk Factors
Scientists are still researching the exact causes of endometriosis, but several factors are thought to play a role:
- Hormonal Influence: Estrogen is believed to encourage the growth of endometrial-like tissue.
- Family History: A higher likelihood exists for women with close relatives affected by the condition.
- Immune System Responses: The immune system may not efficiently remove misplaced cells in some cases.
- Retrograde Menstruation: A theory suggesting menstrual fluid flows backward through the fallopian tubes, allowing cells to attach elsewhere.
No single factor explains every case. Healthcare providers consider a combination of elements, including lifestyle, genetics, and hormonal balance, when assessing a diagnosis.
Everyday Habits That May Support Pelvic Health
While lifestyle choices cannot cure endometriosis, certain habits can significantly support general comfort, manage symptoms, and reduce inflammation-related stress in the body. Many health professionals encourage:
- Regular, Gentle Movement: Activities like walking, stretching, or yoga improve circulation, reduce muscle tension in the pelvic region, and can help with pain management.
- Balanced Nutrition: An anti-inflammatory diet rich in fruits, vegetables, whole grains, and omega-3 fatty acids, while limiting processed foods, red meat, and excessive caffeine/alcohol, may help manage inflammation.
- Stress Management: Chronic stress can worsen pain perception and inflammation. Practices such as meditation, deep breathing, or spending time in nature can be beneficial.
- Adequate Sleep: Prioritizing 7-9 hours of quality sleep per night supports overall immune function and hormone regulation.
Integrating these habits into your daily routine can empower you to better manage symptoms and enhance your overall well-being.