Last week, a patient shared a story that embarrassed him more than his pain. He recounted noticing his slipper had fallen off while walking to the mailbox, yet he never felt it happen. Moments like these often begin subtly—perhaps a strange tingling in the toes or a small patch of numb skin. Initially, many dismiss these sensations, attributing them to normal aging or poor circulation. However, over time, these feelings can slowly spread upward, making everyday movements increasingly difficult and uncomfortable. The good news is that understanding what’s happening within your nerves can empower you to protect them, safeguarding your mobility and independence. Towards the end of this article, we’ll touch on a simple daily consideration many older adults overlook that may significantly support nerve health.
What Peripheral Neuropathy Really Means
Peripheral neuropathy refers to damage affecting the peripheral nerves. These vital nerves act like intricate communication cables, forming a vast network that connects your brain and spinal cord to every other part of your body. When these crucial pathways are disrupted, signals struggle to travel effectively. This disruption can manifest as unusual sensations or changes in muscle control.
Many individuals first notice symptoms in their feet. This is often because the nerves in the lower legs are among the longest in the body, making them more susceptible to damage and stress. Common sensations people describe include:
- Tingling: Often likened to tiny electric shocks or “pins and needles.”
- Numbness: Particularly in the toes or soles of the feet, feeling like they’ve “fallen asleep.”
- Burning Sensations: A persistent, uncomfortable heat that often worsens at night.
- Weakness: A noticeable loss of strength in the legs or hands.
- Reduced Balance or Coordination: Leading to an increased risk of falls.
Research, including insights from organizations like the National Institute of Neurological Disorders and Stroke, highlights that changes in nerve signals can develop very gradually. Due to this slow progression, many people don’t realize what’s occurring until symptoms become more pronounced. Yet, there’s more to the story. Understanding the distinct forms of nerve damage can reveal why symptoms vary so widely from one person to another.
The Three Main Types of Nerve Damage
Peripheral nerve issues generally fall into three primary categories, depending on which specific nerve fibers are affected:
Sensory Nerve Involvement
Sensory nerves are responsible for helping you perceive temperature, pressure, and pain. When these nerves are compromised, individuals may experience:
- Tingling or prickling sensations.
- Loss of feeling in the feet or hands.
- Persistent burning discomfort.
- Extreme sensitivity to even a light touch.
Motor Nerve Involvement
Motor nerves are the conductors of muscle movement. When they are affected, possible signs include:
- Muscle weakness.
- Difficulty lifting the front part of the foot while walking (known as “foot drop”).
- Unwanted cramping or twitching in muscles.
- Reduced grip strength in the hands.
Autonomic Nerve Involvement
Autonomic nerves manage the body’s involuntary processes—functions we don’t consciously control, like heart rate, digestion, and sweating. Examples of issues when these nerves are affected include:
- Changes in sweating patterns (e.g., excessive sweating or reduced sweating).
- Digestive discomfort (e.g., bloating, constipation, or diarrhea).
- Sensations of an irregular heart rhythm.
- Bladder or bowel control changes.
Here’s a simple comparison that helps many patients grasp the distinctions:
| Nerve Type | What It Controls | Possible Signs |
|---|---|---|
| Sensory nerves | Feeling and sensation | Tingling, numbness, burning |
| Motor nerves | Muscle movement | Weakness, cramps, walking difficulty |
| Autonomic nerves | Automatic body functions | Digestive issues, sweating changes |
Knowing which specific nerves are involved helps healthcare professionals better understand symptom patterns and tailor treatment. But the next question many people ask is often even more critical.
What Actually Causes Nerve Damage to Begin With?
A range of health conditions and lifestyle factors can detrimentally affect nerve function. Some of these develop insidiously over many years, which explains why symptoms often emerge later in life. The most common contributing factors include:
- Diabetes and long-term blood sugar imbalance: The leading cause worldwide.
- Vitamin deficiencies: Particularly a lack of Vitamin B12.
- Certain infections: Such as shingles or Lyme disease.
- Autoimmune conditions: Where the immune system mistakenly attacks nerve tissue.
- Long-term alcohol use: Can be toxic to nerves.
- Side effects from some medications: Certain chemotherapy drugs, for example.
- Physical nerve compression: Like carpal tunnel syndrome or spinal disc problems.
- Inherited nerve conditions: Genetic predispositions.
Studies consistently highlight that diabetes-related nerve damage is the most prevalent contributor globally. However, a crucial point many people don’t realize is that multiple factors can often occur simultaneously. For instance, a mild vitamin deficiency combined with circulation problems may significantly increase nerve vulnerability. This underscores precisely why paying close attention to early warning signs is so vital.
Early Signs That Should Not Be Ignored
In clinical practice, many patients voice the same regret: “I wish I had paid attention sooner.” Peripheral nerve symptoms frequently follow a predictable pattern, typically beginning subtly in the feet. The common progression reported by patients often looks like this:
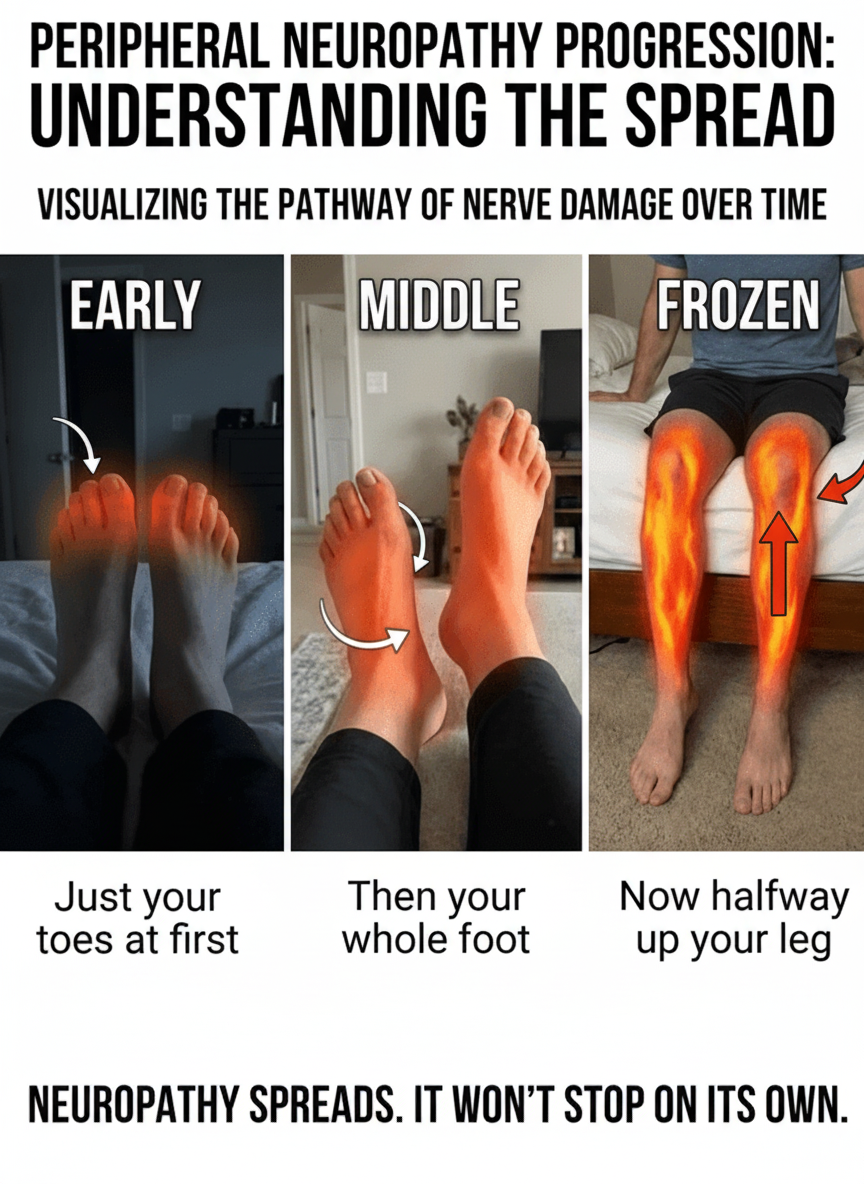
- First stage: Mild, intermittent tingling in the toes.
- Second stage: Numbness begins to spread across the bottom of the foot.
- Third stage: Sensations of numbness, tingling, or burning start to spread gradually upward into the ankles and lower legs.
Recognizing these early stages can make a significant difference in managing the condition and preserving your quality of life.