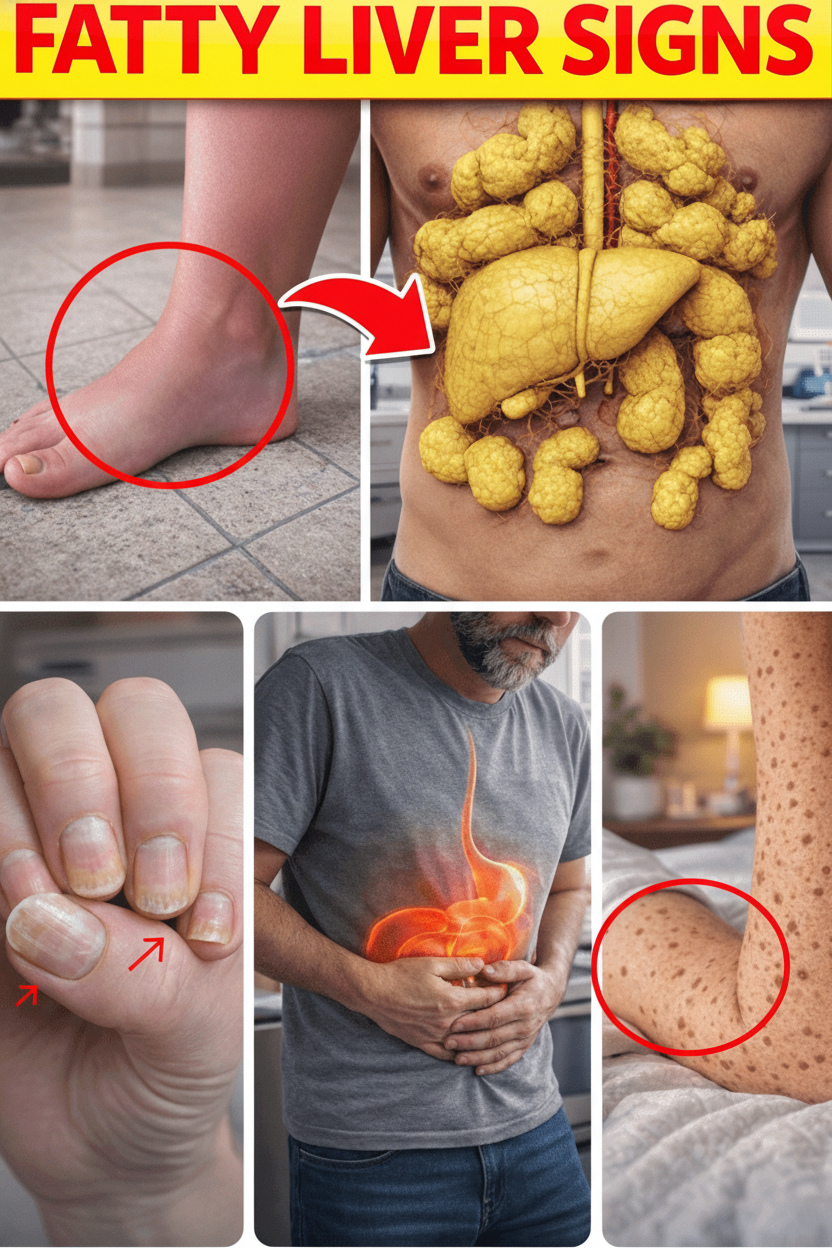
10 Silent Warning Signs of Fatty Liver Disease (MASLD) You Must Not Overlook
Once known as Non-Alcoholic Fatty Liver Disease (NAFLD), this prevalent condition is now officially termed Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD). It stands as one of the globe’s most widespread chronic liver ailments, impacting a significant portion of the adult population—approximately 25-30%. The insidious nature of MASLD lies in its tendency to progress silently for extended periods, often without any noticeable symptoms. This stealthy progression makes it particularly hazardous: by the time distinct warning signs manifest, considerable liver damage, such as inflammation, fibrosis, or even early-stage cirrhosis, may have already taken root.
Many individuals unknowingly experience early-to-mid-stage symptoms of MASLD, frequently dismissing them as consequences of stress, the natural aging process, insufficient sleep, or merely being out of condition. Below, we outline 10 crucial symptoms that are commonly reported. Recognizing these signs, particularly if they are persistent or gradually worsening, should prompt immediate attention. It becomes imperative to undergo comprehensive liver function tests (including ALT, AST, GGT, and bilirubin levels) and diagnostic imaging like an abdominal ultrasound or a FibroScan to assess your liver health.
Understanding the Key Symptoms of MASLD
1. Persistent, Unexplained Fatigue
Experiencing a profound sense of tiredness or consistently low energy levels, even after achieving 8 or more hours of sleep, is a common indicator. This fatigue is often described as feeling “heavy” or utterly “drained,” and it doesn’t alleviate with rest.
- Why it’s common: When the liver is inflamed due to fat accumulation, its ability to efficiently metabolize energy and perform vital detoxification processes is compromised, leading to systemic exhaustion.
2. Dull Ache or Sensation of Fullness in the Upper Right Abdomen
A mild, persistent discomfort or a feeling of heaviness and fullness beneath the right rib cage – the anatomical location of your liver – can signal an issue. This sensation often intensifies following the consumption of fatty foods.
- Why it’s common: An enlarged liver, burdened by excess fat, can stretch the Glisson’s capsule, the protective membrane encasing it, causing this characteristic pain or pressure.
3. Unexplained Weight Gain or Stubborn Belly Fat
Many individuals report gaining weight without significant alterations to their diet or exercise routine, particularly noticing increased fat accumulation around the midsection – often referred to as “belly fat that simply won’t budge.”
- Why it’s common: Insulin resistance, a primary underlying factor in the development of MASLD, encourages the body to store fat more readily, especially around vital organs like the liver.
4. Changes in Urine and Stool Color
Observe if your urine appears unusually dark, resembling the color of tea or cola. Concurrently, stools might become uncharacteristically light, grayish, or even float, indicating potential digestive issues.
- Why it’s common: These changes often point to impaired bile flow, a critical digestive fluid produced by the liver. When liver function is compromised, bile production and excretion can be disrupted.
5. Generalized Itchy Skin Without a Rash
Experiencing widespread itching, particularly noticeable on the palms of your hands, soles of your feet, back, or arms, without any visible rash or skin irritation. This symptom frequently intensifies during nighttime hours.
- Why it’s common: A buildup of bile salts in the bloodstream, a consequence of impaired liver function, can accumulate under the skin and irritate nerve endings, leading to persistent itching.
6. Cognitive Difficulties: Brain Fog, Concentration Issues, or Mild Memory Loss
Individuals may describe feeling mentally “slowed down,” experiencing forgetfulness, or struggling to maintain focus. These cognitive impairments are sometimes referred to as mild “hepatic encephalopathy” in their nascent stages.
- Why it’s common: When the liver is not functioning optimally, it struggles to efficiently filter toxins from the bloodstream. These accumulated toxins can then affect brain function, leading to subtle neuroinflammation and cognitive symptoms.
7. Vascular Changes: Spider Angiomas or Red Palms
The appearance of small, red, spider-like blood vessels (spider angiomas) on the chest, face, or arms, or palms that exhibit a distinct bright redness (known as palmar erythema), can be a visual cue.
- Why it’s common: Liver dysfunction can disrupt the metabolism of hormones and alter blood vessel tone, leading to these characteristic vascular changes on the skin.
8. Tendency for Easy Bruising or Frequent Nosebleeds
Noticing that you bruise easily from minor impacts or experiencing nosebleeds that are more frequent and take an extended time to cease can be a concern.
- Why it’s common: A compromised liver produces fewer essential clotting factors necessary for blood coagulation, increasing the likelihood of bleeding and bruising.
9. Swelling in Extremities or Abdomen (Edema/Ascites)
Observing puffiness in the ankles or legs, particularly towards the end of the day, or experiencing abdominal bloating that feels uncomfortably tight, can indicate fluid retention. In more advanced stages, this is known as edema (in extremities) or ascites (in the abdomen).
- Why it’s common: Liver impairment can lead to portal hypertension (increased pressure in the veins leading to the liver) and reduced production of albumin, a protein that helps keep fluid within blood vessels. Both factors contribute to fluid leakage into surrounding tissues.
10. Yellowing of Skin or Eyes (Jaundice)
A yellow tint appearing in the whites of your eyes or on your skin, even if subtle and initially only noticeable under natural light, is a critical symptom known as jaundice. While often a late sign, it warrants immediate medical attention.
- Why it’s common: Jaundice occurs when the liver is unable to properly process and excretes bilirubin, a yellow pigment formed from the breakdown of red blood cells, leading to its accumulation in the body.
When to Seek Medical Advice: An Urgency Guide for Liver Health
Understanding when to consult a healthcare professional is paramount for managing liver health. This guide outlines different levels of urgency based on the severity and combination of symptoms:
-
Emergency (Seek immediate care / same day):
- Sudden, intense abdominal pain accompanied by vomiting and noticeable yellowing of the skin or eyes.
- Experiencing confusion, extreme exhaustion, or episodes of fainting, which could indicate acute liver failure.
-
Urgent (Consult within days):
- Persistent pain or discomfort in the upper-right abdomen combined with significant fatigue and any degree of yellowing.
- New or worsening swelling in the abdomen or legs, especially if accompanied by shortness of breath.
-
Prompt (Schedule within 1–2 weeks):
- Ongoing fatigue, discomfort in the upper-right quadrant, persistent itching, and changes in urine or stool color.
- Unexplained weight gain coupled with any two to three other symptoms from the list above.
-
Routine Check (Proactive screening, even without symptoms):
- If you have risk factors such as obesity, type 2 diabetes, metabolic syndrome, elevated triglyceride levels, or a history of significant alcohol consumption, it is highly advisable to proactively discuss liver enzyme tests (ALT/AST) and non-invasive imaging (ultrasound or FibroScan) with your doctor every 1-2 years. Early detection is key to preventing severe liver damage.
The Bottom Line: Fatty liver disease, or MASLD, seldom presents with obvious early warning signs. However, the 10 symptoms detailed above represent some of the most reliable indicators reported by individuals eventually diagnosed with MASLD, its more severe form NASH (non-alcoholic steatohepatitis), or advanced stages of liver fibrosis. It is crucial to understand that when several of these signs endure for more than 2-4 weeks – particularly a combination of fatigue, upper-right abdominal discomfort, itching, and dark urine – they should never be dismissed as merely “part of aging.”
Fortunately, detecting fatty liver disease in its nascent stages is often straightforward. A combination of basic blood tests (like liver enzymes and GGT) and non-invasive imaging techniques (such as an ultrasound or FibroScan) can provide an early diagnosis. This early intervention is vital because, at this point, significant lifestyle modifications alone can frequently reverse the condition or dramatically slow its progression. Listen to your body and trust persistent changes; proactive steps taken now can prevent severe outcomes like cirrhosis, liver failure, or the eventual need for a liver transplant.
Immediate Action Step: Tonight, take a moment to gently check your upper-right abdomen for any subtle ache or pressure. Additionally, review the list of symptoms provided and make a note of any persistent changes you’ve been experiencing, such as unusual fatigue, unexplained itching, or alterations in your urine or stool color. Early awareness and action are your best defense against the progression of Metabolic Dysfunction-Associated Steatotic Liver Disease.