Silent Threats: 7 Overlooked Lacunar Stroke Warning Signs for Adults Over 60 (Don’t Miss #4)
Lacunar strokes present a unique challenge, frequently developing subtly in adults over 60. Unlike more dramatic major strokes, these often affect deeper brain regions without immediate, severe symptoms. It’s common for individuals to dismiss subtle shifts—such as minor balance problems or transient weakness—as merely part of the aging process. This oversight allows cumulative damage to small blood vessels to progress unnoticed. These “silent” cerebrovascular events, if left unaddressed, significantly elevate the risk of impaired mobility, cognitive decline, and a loss of personal independence.
However, early recognition of these patterns is crucial for effective vascular health management. It’s imperative to pay close attention, especially to one particular sign (number 4 on our list), which is so frequently misattributed to “just getting older” that many only seek medical attention once its impact has become significant.
Why Lacunar Strokes Pose a Unique Danger and Are Often Missed
These strokes specifically arise when small, penetrating arteries deep within the brain become obstructed. This blockage is frequently linked to chronic conditions such as uncontrolled high blood pressure, diabetes, and other underlying vascular diseases. These minor blockages, or infarcts, eventually form tiny fluid-filled cavities, known as lacunes, within vital brain structures like the basal ganglia, thalamus, or white matter.
Statistical data reveals that lacunar strokes account for a significant proportion—between 25% and 30%—of all ischemic strokes. Furthermore, “silent” lacunar infarcts are detected via MRI in 20-30% of seemingly healthy individuals over the age of 60, with prevalence increasing with advancing age. Distinct from major strokes, individual lacunar events often manifest with no symptoms or only very mild ones, making them easy to overlook initially. However, the cumulative effect of these repeated micro-damages over time can severely impair motor control, sensory perception, balance, and cognitive function. This silent progression is a major contributor to vascular cognitive impairment, significant gait disturbances, an increased risk of falls, and a gradual decline in the ability to perform daily activities.
The encouraging news is that proactive and aggressive management of vascular risk factors—such as maintaining optimal blood pressure levels—can significantly slow the progression of this damage. But the critical question remains: how can one identify these subtle early indicators before they accumulate into more serious issues? Let’s delve into the seven most frequently overlooked warning signs, compiled from extensive clinical observations and findings published in leading neurology journals.
Warning Sign #7: Abrupt, Unexplained Unilateral Sharp, Stabbing, or Burning Pain
Envision experiencing a sudden, intense burning or electric-shock sensation in your foot, hand, or anywhere along one side of your body, without any apparent injury or clear external cause. This symptom can also manifest as extreme sensitivity to touch, where even light contact causes significant pain—a condition known as allodynia. Such sensations frequently originate from a lacunar infarct located in the thalamus, a critical region of the brain responsible for relaying sensory information.
This phenomenon, often termed central post-stroke pain or thalamic pain syndrome, affects a specific group of stroke survivors and can evolve into a chronic condition. Research consistently shows its occurrence in a notable percentage of cases involving thalamic damage. Disturbingly, it is often mistakenly diagnosed as peripheral neuropathy or various forms of arthritis. Should you encounter such abrupt, unusual, and one-sided sensory experiences, it is crucial not to postpone seeking medical advice; a thorough evaluation by a healthcare professional is essential.
Warning Sign #6: Unexplained Severe Abdominal or Flank Discomfort
While uncommon, there are documented instances where individuals experiencing lacunar strokes report severe, wave-like abdominal or flank pain, strikingly similar to symptoms of kidney stones or other gastrointestinal problems. Crucially, in these cases, standard diagnostic tests for kidney or abdominal issues—such as scans for stones or cultures for infection—yield negative results. This unusual symptom presentation can stem from disturbances in the pain signaling pathways located in the thalamus or brainstem.
When conventional investigations for abdominal discomfort fail to identify a cause, this atypical pain can sometimes lead physicians to pursue advanced brain imaging, which subsequently uncovers the underlying lacunar stroke.
Warning Sign #5: Transient Weakness or Clumsiness Affecting One Limb
Imagine your hand suddenly feeling unusually heavy, tools slipping from your grasp, or one leg briefly dragging as you walk, only for these sensations to quickly subside. These could be indicators of a pure motor lacunar stroke, impacting critical areas such as the internal capsule or pons. Such episodes typically mimic transient ischemic attacks (TIAs), lasting anywhere from a few minutes to several hours, and are observed in a significant percentage (50-60%) of symptomatic lacunar stroke cases.
Unfortunately, many individuals tend to brush off these fleeting symptoms, attributing them to simple fatigue or muscle strain. However, neurological research underscores the vital importance of seeking immediate medical evaluation, even if the symptoms resolve rapidly. These seemingly minor and temporary disturbances are crucial signals of vulnerable brain tissue that requires urgent attention.
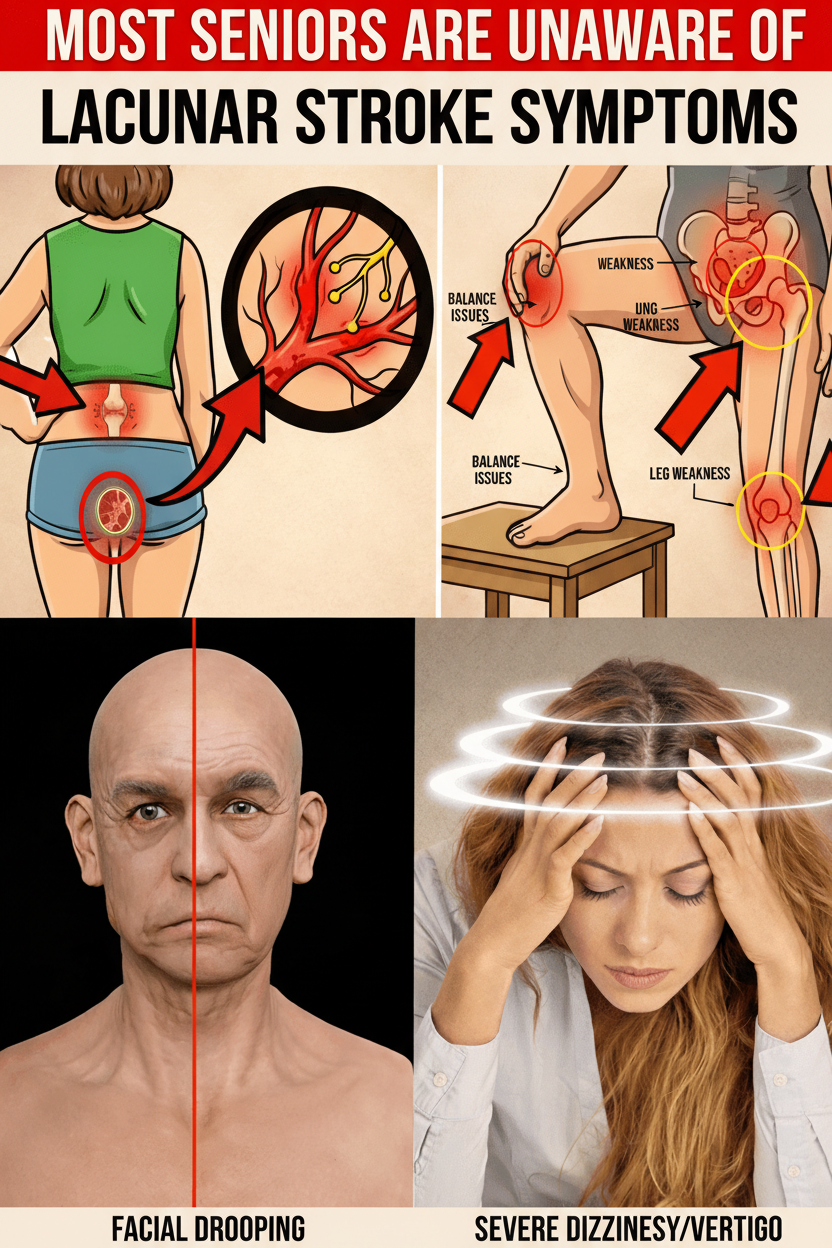
Warning Sign #4: Progressive Balance Issues and Unexplained Falls (The Most Commonly Overlooked)
This particular sign is arguably the most frequently misidentified. It encompasses symptoms such as a shuffling gait, a sensation of being “stuck” or frozen, taking unusually small steps, experiencing difficulty or “freezing” when turning, or suffering frequent stumbles that are often casually dismissed as consequences of normal aging or arthritis. These issues are often indicative of vascular parkinsonism, a condition resulting from lacunar infarcts in critical areas like the basal ganglia or white matter.
Characteristic features include a pronounced emphasis on lower-body difficulties, notably the absence of the classic tremor associated with Parkinson’s disease, and a limited response to standard Parkinson’s medications. Walking becomes notably slower and more cautious, and the ability to perform multiple tasks simultaneously (such as walking while talking) significantly deteriorates, leading to an increased incidence of falls. Research published in movement disorder journals highlights that vascular causes contribute to up to 30% of parkinsonism cases in older adults, making it a significant, yet often overlooked, factor. Family members are frequently the first to observe these subtle but impactful changes.
A critical self-assessment question to consider: how consistent and steady has your walking been recently? Any increasing pattern of unexplained stumbles or balance problems absolutely warrants a comprehensive neurological evaluation and potentially advanced brain imaging. But there’s more to uncover; the subsequent warning signs integrate into daily life in ways that might surprise you.