Prostate cancer stands as a leading malignancy among men globally, yet its initial development frequently occurs without clear symptoms. Many individuals mistakenly attribute subtle shifts in their urinary patterns or energy levels to the natural progression of aging, only to later realize these could have been crucial indicators. Such a delay can significantly impact treatment success, as prompt recognition paves the way for early medical consultation. Reputable sources like the American Cancer Society and Mayo Clinic emphasize that swiftly identifying these changes dramatically enhances the likelihood of addressing potential problems before they become advanced. However, monitoring your health doesn’t have to be a source of anxiety; instead, it can be a powerful act of self-care. This comprehensive guide will systematically explore the primary warning signs of prostate cancer, elucidate their causes, and provide actionable steps you can implement today. Read on to discover a straightforward checklist designed to help you identify potential patterns early on.
Understanding Prostate Cancer and Why Symptoms Often Appear Late
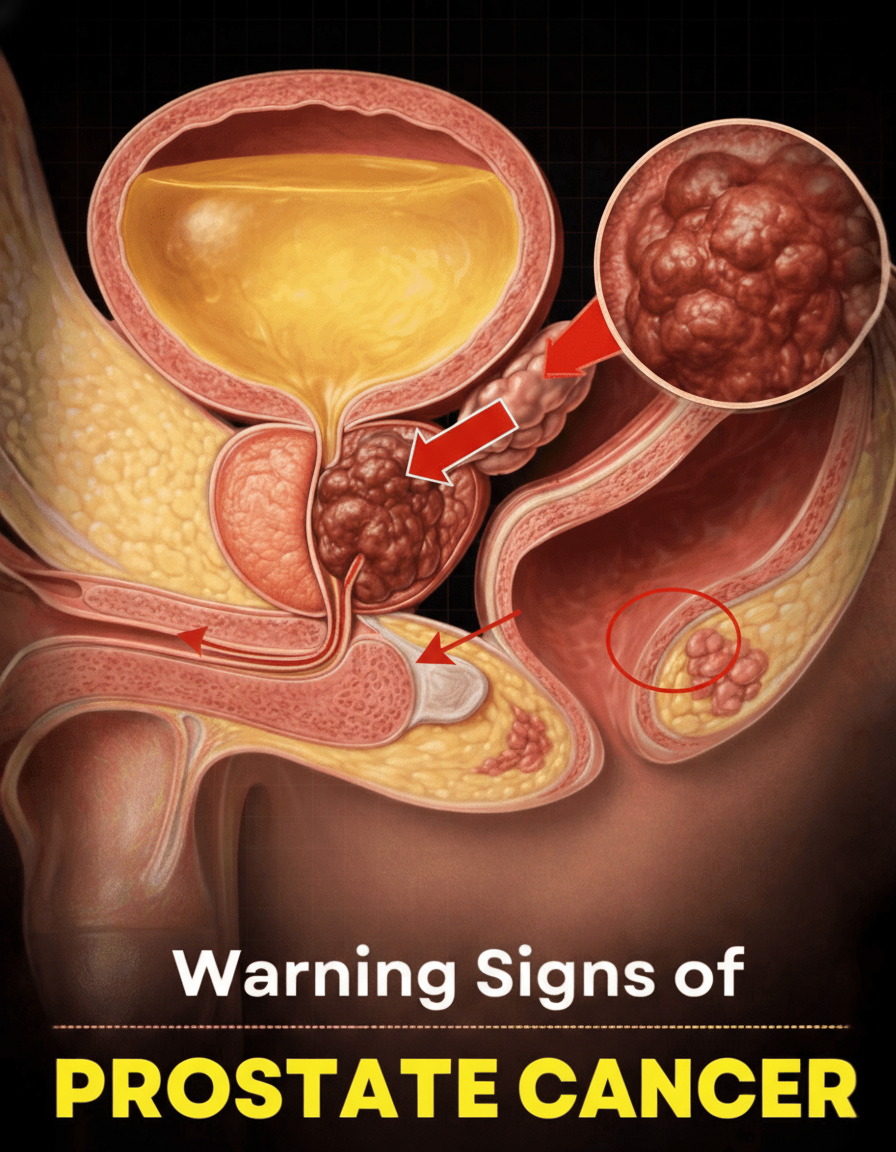
The prostate, a small gland situated beneath the bladder, is integral to male reproductive health. Prostate cancer originates when cells within this gland begin to multiply without control. Frequently, especially during its nascent stages, the disease presents no discernible symptoms—highlighting the critical importance of regular screening conversations with your healthcare provider once you reach a certain age. As the cancerous growth expands or impinges on adjacent tissues, symptoms typically manifest as urinary issues, given that the prostate gland encircles the urethra, the conduit for urine. Studies consistently show that alterations in urinary function are among the most commonly reported initial indicators. Nevertheless, it’s crucial to remember that these changes can also arise from non-cancerous conditions, such as benign prostatic hyperplasia (BPH). However, the full spectrum of potential signs extends beyond just urinary complaints. Let’s delve into these indicators, categorized for clarity, to help you discern what might necessitate a medical evaluation.
Common Urinary Symptoms: The Earliest and Most Frequent Clues
For many men, changes in urination are often the first and most noticeable signs, primarily because an enlarging prostate can exert pressure on the urethra. Pay close attention to these potential indicators:
- A noticeable increase in urination frequency, particularly needing to wake up multiple times during the night (known as nocturia).
- A urine stream that is weak, hesitant, or frequently stops and starts, often feeling less forceful or taking longer to initiate.
- Struggling to begin the flow of urine or requiring effort to maintain it.
- An abrupt and intense need to urinate, sometimes accompanied by small, involuntary leaks.
- The persistent feeling that your bladder hasn’t fully emptied after urinating.
These symptoms typically develop subtly over time, making it easy to adjust without recognizing an underlying issue. However, if you observe these changes persisting for several weeks, documenting them is advisable. Consider this brief self-assessment:
- Are you urinating more than eight times within a 24-hour period?
- Do you find yourself waking up two or more times each night to use the restroom?
- Has the strength of your urine flow significantly decreased over the past few months?
Keeping a simple record of these patterns, perhaps in a note on your smartphone, can provide valuable information to discuss with your doctor.
Pain or Discomfort During Urination
Although not always present in the initial stages, some men may encounter:
- A burning or stinging sensation experienced while passing urine.
- The presence of blood in the urine (medically termed hematuria)—which might manifest as a pink, red, or even cola-like discoloration. This symptom invariably warrants immediate medical assessment. While blood in urine is never considered normal and can signal various conditions such as infections or kidney stones, it is also a well-recognized red-flag indicator for potential prostate issues, as highlighted by health authorities like the Mayo Clinic.
Sexual and Reproductive Changes to Be Aware Of
Given the prostate’s integral role in ejaculation and overall sexual function, cancerous developments or associated alterations can manifest as:
- Challenges in achieving or sustaining an erection (known as erectile dysfunction).
- Discomfort or pain during or immediately following ejaculation.
- The appearance of blood in semen, which may present as a reddish or brownish tint.
- A diminished sex drive or general loss of sexual interest, sometimes connected to profound fatigue or hormonal imbalances.
While these symptoms can often coincide with other age-related physiological changes or existing medical conditions, their presence—particularly when observed in conjunction with urinary problems—should prompt a thorough medical review.
Advanced Signs: Pelvic, Back, or Bone Pain
Should the cancer progress to more advanced stages and metastasize to bones or adjacent regions, you might experience:
- Chronic pain in the lower back, hips, or pelvic area that does not subside.
- Aching in the bones that intensifies during nighttime hours or with physical activity.
- In infrequent cases, weakness in the legs or difficulty with gait (walking), which could signal potential spinal cord compression.
These are more critical indicators, typically associated with advanced prostate disease, and therefore, any enduring discomfort should not be overlooked.
General Symptoms That Affect the Whole Body
Prostate cancer, like other malignancies, can induce systemic effects that impact the entire body. These include:
- Significant and unexplained weight loss, occurring without any intentional changes to diet or exercise routines.
- Profound and persistent fatigue or generalized weakness that does not alleviate even with adequate rest.
- A noticeable reduction in appetite.
These broader symptoms frequently manifest in conjunction with other specific indicators and often arise from the body’s overall response to the presence of cancer.